The Silent Epidemic: Understanding and Addressing Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD)
A 50-year-old male professional recently visited a hospital complaining of weight gain and fatigue. He had previously been diagnosed with diabetes and hyperlipidemia and was undergoing medication. An abdominal ultrasound revealed fatty liver disease. This case highlights a growing concern in modern healthcare: the rise of metabolic dysfunction-associated steatotic liver disease (MASLD), a condition rapidly gaining attention as a significant public health issue.
From NAFLD to MASLD: A Paradigm Shift
Traditionally known as non-alcoholic fatty liver disease (NAFLD), the condition is now being reframed as MASLD. This shift reflects a deeper understanding of its connection to metabolic disorders. MASLD is characterized by fat accumulation in the liver, coupled with inflammation, and is closely linked to conditions like diabetes, obesity, and hyperlipidemia. This evolution in understanding emphasizes that MASLD isn’t simply a liver problem, but a systemic metabolic issue.
According to experts, MASLD carries a risk of progressing to liver fibrosis and cirrhosis, and also increases the risk of cardiovascular disease. Early diagnosis and management are crucial to prevent severe liver damage and associated health complications.
Identifying MASLD: A Two-Step Approach
Diagnosing MASLD involves a two-step process. The initial screening utilizes the ‘Fibrosis-4’ score, a blood test-based assessment that evaluates the risk of liver fibrosis based on age and platelet count. A score below 1.3 suggests a low risk of progressive fibrosis, allowing for management within a primary care setting. However, criteria may vary based on factors like the presence of diabetes, age, and younger patients. Scores exceeding 2.67 warrant consultation with a liver specialist.
For those identified as moderate to high risk, further evaluation involves non-invasive tests like liver fibrosis scans or MRI-based elastography to assess the degree of fibrosis more accurately.
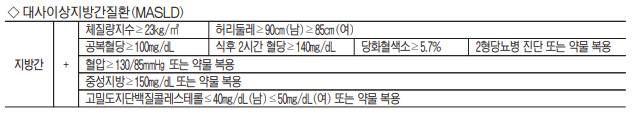
Cardiometabolic Risk Factors: The Key to Understanding MASLD
The presence of at least one cardiometabolic risk factor is now considered essential for diagnosing MASLD. These factors include indicators of metabolic syndrome, highlighting the interconnectedness of liver health and overall metabolic function.
The Growing Prevalence of MASLD
With the increasing prevalence of obesity and diabetes, MASLD is also on the rise. Current estimates suggest a prevalence ranging from 25% to 47%, varying based on testing methods and criteria. The condition is more common in men and tends to increase in women after menopause.
The Importance of Early Intervention
While MASLD progresses relatively slowly, its association with worsening metabolic disease and increased cardiovascular risk underscores the importance of early diagnosis and management. Experts recommend regular check-ups every 2-3 years, coupled with lifestyle modifications and, when necessary, medication.
Weight loss is considered the most important first step in reversing MASLD. A consistent approach to diet, balanced nutrition, and regular exercise can help restore liver health and return it to a normal state.
Pro Tip:
Compact, consistent changes to your lifestyle are more sustainable than drastic overhauls. Focus on incorporating more fruits and vegetables into your diet, reducing processed foods, and finding physical activities you enjoy.
FAQ
What is the difference between NAFLD and MASLD? MASLD is a more precise term that emphasizes the link between fatty liver disease and underlying metabolic dysfunction. It acknowledges that the condition is not simply a result of factors other than alcohol, but is deeply connected to metabolic disorders.
How is the Fibrosis-4 score used? The Fibrosis-4 score is a simple blood test that helps assess the risk of liver fibrosis. It’s used as an initial screening tool to determine if further investigation is needed.
What are cardiometabolic risk factors? These are factors that increase the risk of both heart disease and metabolic disorders, such as diabetes, obesity, and high blood pressure.

