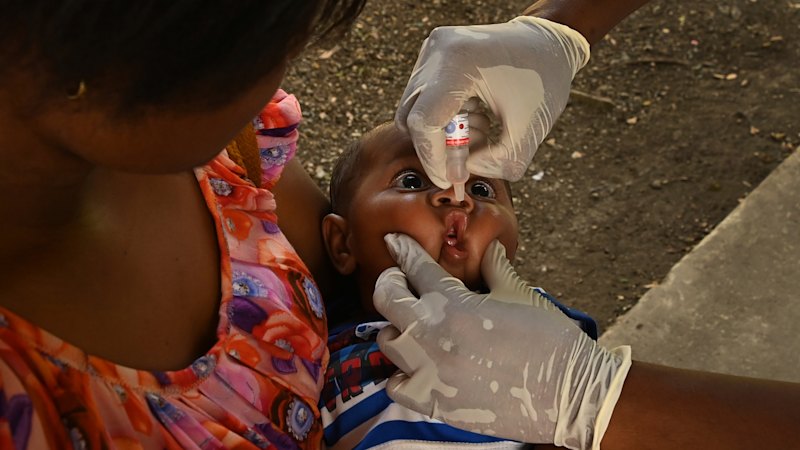
The New Frontier of Polio Eradication: Lessons from the Global Frontline
The recent resurgence of polio in regions previously declared polio-free serves as a stark reminder that eradication is not a finish line, but a continuous process of vigilance. When vaccination rates dip, the void is quickly filled by ancient killers. The struggle in Papua New Guinea—where health workers navigate helicopters, rafts, and hiking trails to reach remote villages—highlights a broader global trend: the fight against polio has shifted from a battle of medicine to a battle of logistics, and trust.

Some outbreaks are caused by vaccine-derived poliovirus
. This occurs when the weakened virus used in oral vaccines circulates in under-vaccinated communities with poor sanitation, eventually mutating back into a form that can cause paralysis.
Beyond the Needle: The Rise of Wastewater Surveillance
One of the most significant shifts in modern epidemiology is the move toward environmental monitoring. We no longer have to wait for a child to present with paralysis—a late-stage clinical symptom—to know a virus is present. Wastewater surveillance, as utilized by the Peter Doherty Institute, allows scientists to detect the genetic fingerprints of poliovirus in sewage systems before a single human case is reported.
This “early warning system” is becoming a blueprint for global health security. By sampling wastewater in transit hubs and border cities, health authorities can trigger rapid-response vaccination campaigns to “ring-fence” an outbreak. This proactive approach reduces the likelihood of international importation, protecting countries that maintain high vaccination levels but remain vulnerable to travelers.
The “Zero-Dose” Dilemma and Pandemic Aftershocks
The global health community is currently facing a crisis of zero-dose children
—those who have never received a single routine immunization. Between 2023 and 2025, an estimated 12.3 million children fell into this category. This gap is largely a legacy of the COVID-19 pandemic, where lockdowns and disrupted healthcare systems halted routine childhood vaccinations.
The danger is not just the absence of a vaccine, but the creation of “immunity gaps.” When a significant percentage of a population is unvaccinated, the community loses its herd immunity, providing a playground for viruses to mutate and spread. In some provinces of Papua New Guinea, polio coverage has fallen below 40 per cent, creating a high-risk environment for both the local population and neighboring nations.
Combatting vaccine hesitancy requires “proper awareness.” As noted by frontline nurses, explaining the why behind a campaign—rather than just the how—is the most effective way to move a skeptical community toward acceptance.
The Evolution of Vaccine Technology: nOPV2
To combat the risk of vaccine-derived outbreaks, the scientific community is transitioning toward more stable vaccine versions. The traditional Sabin type 2 vaccine, while effective, was prone to mutation. The introduction of the novel oral polio vaccine type 2 (nOPV2) is a game-changer, designed to be genetically more stable and significantly less likely to revert to a paralytic form.
The future of eradication relies on this marriage of better biology and better delivery. Whether it is using drones to bypass broken road networks or deploying community-led “awareness” teams to fight misinformation, the goal is a 95 per cent vaccination rate—the gold standard for stopping transmission.
Global Interconnectedness: No One is Safe Until All Are
The risk of polio importation is a reality for every nation. Even in developed countries, falling childhood vaccination rates in various age groups create pockets of vulnerability. As seen in recent detections in Australian wastewater, the virus can travel across borders via unvaccinated travelers.
The success of the response in Papua New Guinea, which has already vaccinated more than two million children, is not just a local victory; it is a protective shield for the rest of the world. The trend is clear: global health security is only as strong as the weakest health system in the most remote village.
For more on how emerging diseases are monitored, explore our guide on the future of genomic sequencing or visit the World Health Organization for latest eradication data.
Frequently Asked Questions
The oral polio vaccine (OPV) contains a weakened virus. In rare cases, in areas with very low vaccination rates and poor sanitation, this weakened virus can circulate and mutate into a vaccine-derived poliovirus (cVDPV) that can cause paralysis. This is why the world is moving toward the more stable nOPV2 and inactivated polio vaccines (IPV).
Why is wastewater testing important?
Wastewater testing detects the virus in the community before people gain sick. It provides an unbiased snapshot of viral circulation, allowing health officials to launch vaccination drives before a clinical outbreak occurs.
What are “zero-dose” children?
Zero-dose children are those who have not received any doses of the most basic childhood vaccines. They represent the most vulnerable populations and are the primary targets for catch-up immunization campaigns.
Join the Conversation
Do you believe global health systems are doing enough to prevent the return of eradicated diseases? Share your thoughts in the comments below or subscribe to our newsletter for deep dives into global health security.