Hantavirus Outbreaks: What the Cruise Ship Cluster Reveals About Future Risks—and How to Stay Ahead
The recent hantavirus cluster aboard the MV Hondius, with 11 confirmed cases and three deaths, has exposed critical gaps in global health preparedness. As travel continues to rebound post-pandemic, experts warn that zoonotic diseases like hantavirus—once confined to rural regions—are increasingly turning up in unexpected places. What does this mean for future outbreaks? And how can individuals, healthcare systems and policymakers mitigate risks? Here’s what the science, data, and recent events tell us.
— ### **The New Face of Hantavirus: From Forests to Cruise Ships** #### **A Disease That Breaks the Rules** For decades, hantavirus was considered a rural threat, primarily spread through contact with rodent urine, droppings, or saliva in forests, farms, or abandoned buildings. But the Andes virus (ANDV)—the strain behind the cruise ship outbreak—has defied expectations. Unlike most hantaviruses, ANDV is one of the few known to spread person-to-person, particularly in close-contact settings.
Did you know? The Andes virus is the only hantavirus confirmed to transmit between humans. Before this cruise ship cluster, cases were mostly linked to household or healthcare worker exposure in South America. The ship outbreak suggests the virus can spread more efficiently in confined, high-density environments like cruise liners, hospitals, or even long-haul flights.
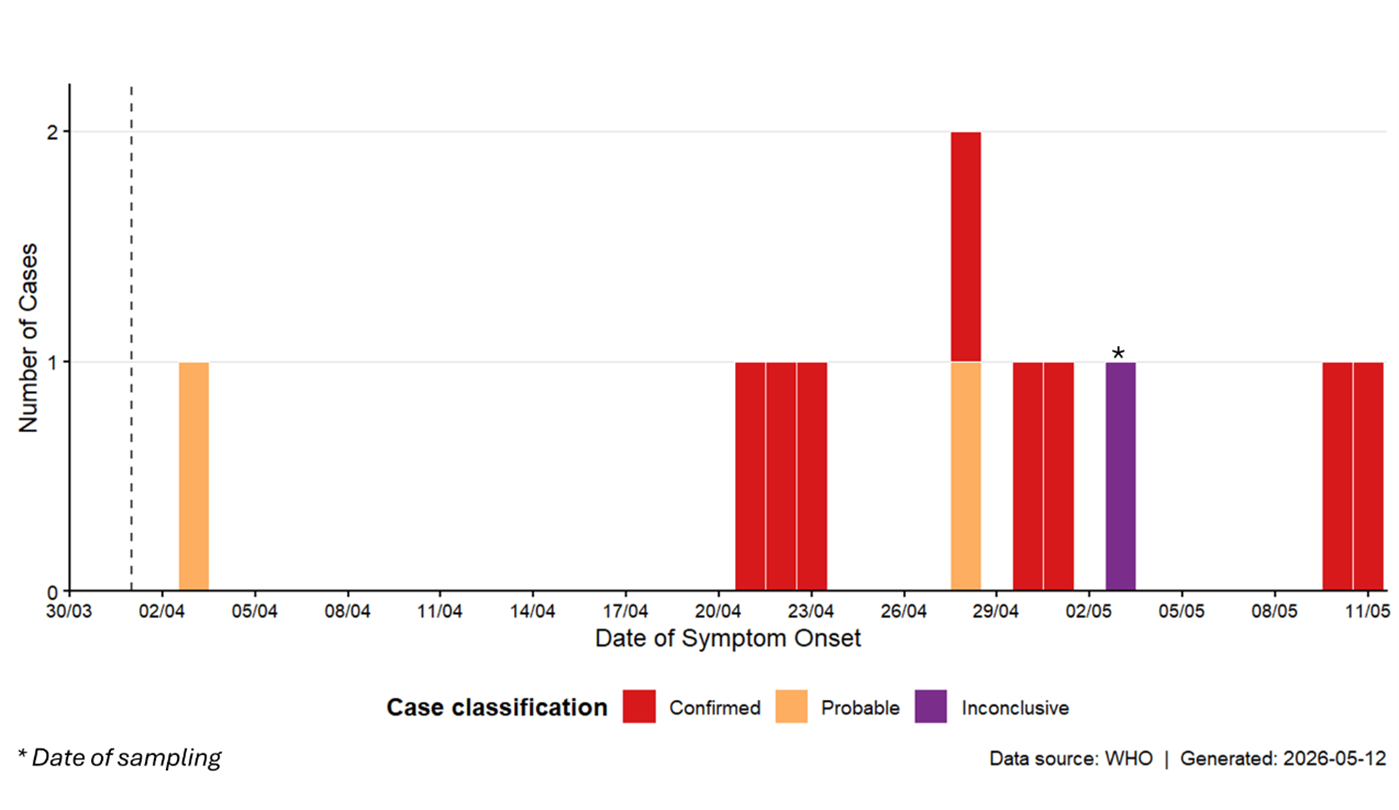
#### **How Did It Happen? Tracing the Cruise Ship Cluster** The investigation into the MV Hondius outbreak points to a zoonotic spillover event—likely from a passenger who contracted the virus before boarding, possibly during birdwatching or outdoor activities in Argentina or Chile, where ANDV is endemic. Genetic sequencing reveals the virus mutated minimally among cases, suggesting it spread efficiently among passengers once onboard. Key transmission factors on the ship: ✔ **Close quarters** – Cabins, dining halls, and shared spaces increased exposure. ✔ **Prolonged exposure** – Passengers spent weeks in close contact with infected individuals. ✔ **Asymptomatic spread** – Some cases tested positive but showed no symptoms, complicating containment. Data in focus: – **Case fatality rate (CFR):** 27% (3 deaths out of 11 cases), aligning with the 40-50% CFR seen in severe hantavirus pulmonary syndrome (HPS) cases in the Americas. – **Average passenger age:** 65, a high-risk group due to weaker immune responses. – **Genetic similarity:** Near-identical viral sequences across cases suggest a single or limited spillover events followed by human transmission. — ### **Future Trends: Why Hantavirus Could Become More Common** #### **1. Globalization and Zoonotic Spillover** As travel, trade, and urbanization expand, zoonotic diseases (diseases jumping from animals to humans) are on the rise. The WHO estimates that 75% of emerging infectious diseases originate in animals. Hantavirus is no exception. Real-world risks: – **Ecotourism & adventure travel** – Activities like hiking, camping, and birdwatching in endemic regions (e.g., Patagonia, the Andes) increase exposure. – **Climate change** – Warmer temperatures and shifting rodent habitats may expand hantavirus ranges into new areas. – **Urban encroachment** – Cities expanding into rural zones bring humans into closer contact with rodent reservoirs.
Pro Tip: If you’re traveling to hantavirus-endemic regions, avoid disturbing rodent nests (e.g., cleaning attics, handling hay). Use rodent-proof containers for food and dispose of trash properly. Always wash hands after outdoor activities.
#### **2. The Rise of Human-to-Human Transmission in Unlikely Places** Before the cruise ship outbreak, ANDV transmission was rare outside of household or healthcare settings**. But the MV Hondius case proves the virus can spread in: – **Cruise ships** (high-density, enclosed environments) – **Long-haul flights** (where asymptomatic passengers may unknowingly expose others) – **Hospitals** (healthcare workers are at risk if proper PPE isn’t used) Expert warning: > *”This outbreak changes the risk calculus. We can no longer assume hantavirus is just a rural disease. It’s now a travel-associated risk that requires vigilance in both endemic and non-endemic regions.”* — **WHO Disease Outbreak News, May 2026** #### **3. Diagnostic and Treatment Gaps** Despite the severity of hantavirus, no vaccine or specific antiviral treatment exists**. Current management relies on: – **Early ICU care** (mechanical ventilation, fluid management) – **Supportive therapy** (antibiotics for secondary infections, dialysis for kidney failure) – **Extracorporeal membrane oxygenation (ECMO)** in severe cases (used in 20% of survivors) Challenges ahead: – **Delayed diagnosis** – Early symptoms (fever, muscle aches) mimic flu or COVID-19. – **Limited lab capacity** – Many countries lack hantavirus testing infrastructure. – **Asymptomatic carriers** – Some infected individuals may spread the virus unknowingly. Breakthroughs on the horizon: – **Rapid antigen tests** (currently in development) could speed up diagnosis. – **Monoclonal antibodies** are being researched for HPS treatment. – **Vaccine trials** in Argentina and Chile may expand to other regions. — ### **How to Prepare: Lessons from the Cruise Ship Outbreak** #### **For Travelers: Protect Yourself Before, During, and After the Trip** If you’re planning a trip to South America, Europe, or Asia (where hantavirus risks vary), follow these steps: ✅ **Before Travel:** – Check the CDC’s hantavirus risk map (https://news.google.com/rss/articles/CBMiekFVX3lxTE54a0hHNDdXYW1vT1RwSjFVek0yZW01WDAwT0hBdVc2TTNtSV82ZjhNYW9hdURjdWtMOFNuUWNjdkM1Y2pUS1VFcm82aXVmaGE3Z1dpU1FfYXlOMDRjdjRYU3hKbmZiNnVycUJGUHJVT1RlNmFSNFdVeFNR?oc=5(https://www.cdc.gov/hantavirus/geographic.html)) for endemic regions. – Pack a **portable UV sanitizer** for high-touch surfaces (door handles, railings). ✅ **During Travel:** – **Avoid rodent habitats** – Don’t enter caves, abandoned buildings, or dense brush. – **Use insect repellent** (some rodent-borne diseases spread via ticks or fleas). – **Disinfect luggage** after outdoor activities (rodent saliva can linger on clothing). ✅ **After Returning Home:** – Monitor for symptoms (fever, muscle aches, cough) for **up to 8 weeks** post-exposure. – Seek **immediate medical attention** if respiratory distress develops.
Reader Question: *”I took a cruise to the Caribbean last month. Should I be worried?”* Answer: The Andes virus is not endemic in the Caribbean, but if you visited South America before or after, monitor for symptoms. Cruise ships in non-endemic regions have low risk unless a confirmed case is onboard (as with the MV Hondius).
#### **For Healthcare Providers: Recognizing and Responding to Hantavirus** With hantavirus now a travel-associated diagnosis**, clinicians must: – **Consider hantavirus in differential diagnoses** for patients with: – Sudden respiratory distress + flu-like symptoms – Recent travel to endemic regions – Exposure to rodents or confirmed cases – **Isolate suspected cases immediately** (use airborne precautions). – **Report suspected cases** to public health authorities for contact tracing. Clinical red flags: – **Biphasic illness** – Initial flu-like symptoms followed by sudden pulmonary edema**. – **Low platelet count** (thrombocytopenia) in severe cases. #### **For Policymakers: Strengthening Global Health Security** The cruise ship outbreak highlights the need for: 🔹 **Enhanced surveillance** – Airports and ports should screen for febrile travelers from high-risk regions. 🔹 **Rapid response protocols** – Cruise lines and airlines must have infection control plans** for outbreaks. 🔹 **International coordination** – The WHO’s International Health Regulations (IHR) worked in this case, but gaps remain in real-time data sharing**. Policy ask: > *”We need a global early warning system for zoonotic spillovers—one that integrates travel, wildlife, and public health data.”* — **WHO Director-General, Tedros Adhanom Ghebreyesus** — ### **FAQ: Your Burning Questions About Hantavirus Answered**
1. Can hantavirus spread on a plane or in a hotel?
Yes, but it’s rare. The Andes virus spreads through close, prolonged contact with an infected person’s saliva or respiratory droplets. On a plane, risk is low unless someone is symptomatic. Hotels pose minimal risk unless there’s rodent infestation** (which can spread the zoonotic form).
2. Is there a vaccine for hantavirus?
No licensed vaccine exists globally. However, Argentina and Chile use experimental vaccines** in high-risk populations (e.g., healthcare workers, lab staff). Research is ongoing for broader availability.
3. How long should I quarantine if exposed to hantavirus?
The WHO recommends 42 days of active monitoring** for high-risk contacts (e.g., household members, healthcare workers). Low-risk contacts (e.g., casual acquaintances) should self-monitor and seek care if symptoms develop.
4. Can pets or livestock spread hantavirus?
No. Hantavirus is rodent-specific**—dogs, cats, and livestock do not transmit the virus. However, pets can carry rodent fleas or ticks that may spread other diseases.
5. What’s the difference between hantavirus in the Americas vs. Europe/Asia?
In the Americas**, hantavirus causes HPS (hantavirus pulmonary syndrome)**, primarily affecting the lungs. In Europe/Asia**, it causes HFRS (hemorrhagic fever with renal syndrome)**, primarily damaging the kidneys. Only the Andes virus** spreads person-to-person.
— ### **The Bottom Line: A Wake-Up Call for Global Health** The MV Hondius outbreak is a warning sign**—one that suggests hantavirus is evolving into a travel-associated threat**. While the global risk remains low for most people, the potential for future outbreaks in cruise ships, long-haul flights, or even urban settings** cannot be ignored. Key takeaways: ✔ **Travelers** must stay vigilant in endemic regions and monitor symptoms post-trip. ✔ **Healthcare systems** need better diagnostic tools and outbreak response plans. ✔ **Policymakers** must invest in zoonotic disease surveillance** and international coordination.
Final Thought: The next pandemic could start with a single rodent encounter**—followed by human transmission in an unexpected place. The cruise ship outbreak proves we’re not just fighting diseases in the wild anymore. We’re fighting them in airplanes, hotels, and even on vacation**. The question isn’t if another outbreak will happen—but when. Are we ready?
— ### **What You Can Do Next** 🔹 **Stay informed** – Follow updates from the [WHO](https://www.who.int/emergencies/disease-outbreak-news/item/2026-DON601) and [CDC](https://www.cdc.gov/hantavirus/). 🔹 **Plan ahead** – If traveling to high-risk areas, review preventive measures** before departure. 🔹 **Share your thoughts** – Have you or someone you know encountered hantavirus? Comment below**—your experience could help others. 🔹 **Subscribe for more** – Get expert analysis on emerging diseases and travel health [here]. —
🚨 Don’t wait for the next outbreak to prepare. Stay ahead with science-backed health insights—subscribe now! 🚨