Silent Snoring: Why Your Child’s Sleep Could Be Shaping Their Face
Many parents dismiss a child’s snoring as a sign of peaceful sleep. However, it could be an early indicator of obstructive sleep apnea (OSA), a condition increasingly linked to developmental issues and even facial structure. As an ENT specialist, I’m seeing more and more cases where seemingly unrelated problems – learning difficulties, behavioral issues – trace back to disrupted sleep caused by OSA.
The Link Between Sleep Apnea and Facial Development
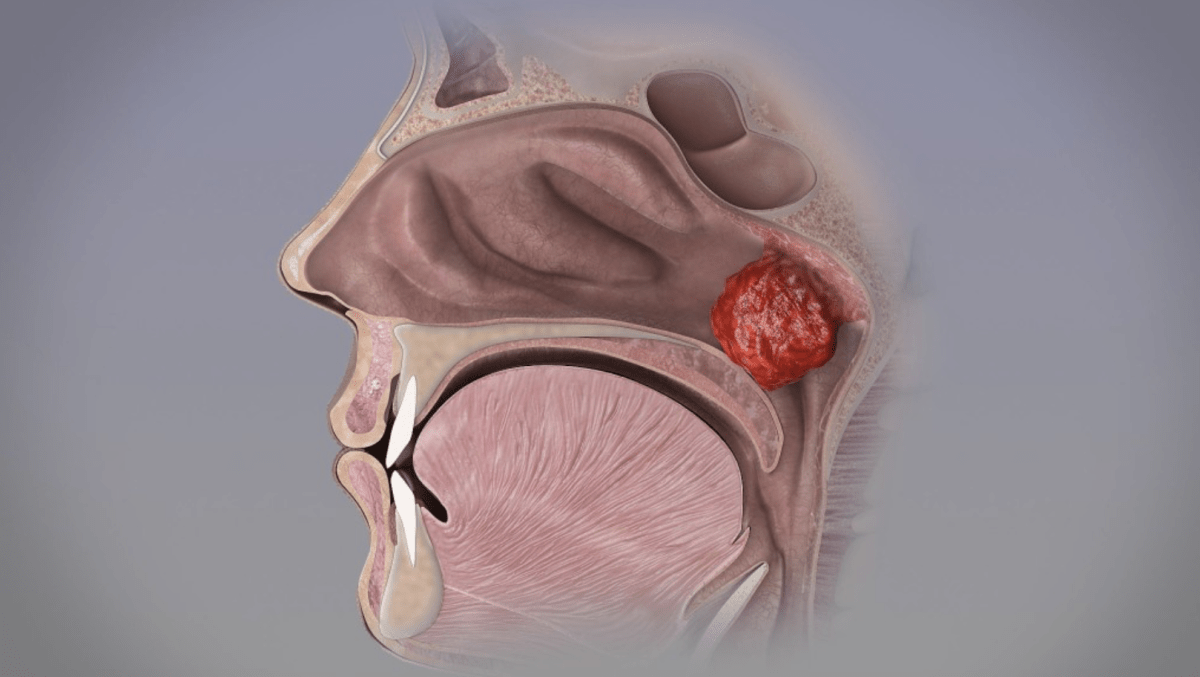
Pediatric obstructive sleep apnea occurs when the upper airway becomes blocked during sleep, leading to pauses in breathing. Enlarged tonsils and adenoids are the most frequent culprits, but factors like obesity and craniofacial abnormalities can also contribute. These repeated breathing interruptions don’t just affect sleep quality; they can physically alter a child’s face.
Chronic mouth breathing, often a consequence of airway obstruction, disrupts the natural balance of facial muscles. This can lead to what’s known as “adenoid facies,” characterized by:
- Upper lip elevation and protruding front teeth
- Poor upper jaw development, resulting in a high-arched palate
- A recessed lower jaw
- An elongated facial appearance with a lack of expression
Recent data suggests that approximately 49.7% of children experience adenoid hypertrophy, a key contributor to OSA. This creates a cycle where mouth breathing, misaligned teeth, and abnormal facial development reinforce each other.
Treatment Options: From Surgery to Orthodontics
For sleep apnea stemming from enlarged tonsils and adenoids, adenotonsillectomy remains the most common and effective treatment. While parents understandably worry about surgery, clinical evidence supports its benefits. A 2025 study showed that children with mild sleep-disordered breathing who underwent adenotonsillectomy experienced a 32% reduction in overall healthcare utilization and a 48% reduction in prescription medication needs within a year.
However, surgery isn’t always necessary. Watchful waiting may be appropriate for mild cases, particularly in children with smaller tonsils. Personalized treatment plans are crucial, considering the location and severity of the airway obstruction. Orthodontic treatment or orofacial myofunctional therapy may also be recommended.
The Rise of Home Sleep Testing
Traditionally, diagnosing sleep apnea required an overnight stay in a sleep lab. Now, home sleep testing is becoming increasingly accessible, offering a more convenient option for many families. Brooklyn ENT & Allergy, for example, provides home sleep testing services, allowing patients to be evaluated in the comfort of their own homes.
Future Trends in Pediatric Sleep Apnea Care
The field of pediatric sleep apnea is evolving rapidly. Several trends are poised to shape future care:
- Sleep Endoscopy: Mount Sinai is utilizing sleep endoscopy, a technique to evaluate complex cases of obstructive sleep apnea.
- Multidisciplinary Approach: ColumbiaDoctors Children’s Health emphasizes a collaborative approach, involving pediatric ENT physicians, obesity experts, and other specialists.
- Personalized Medicine: Treatment plans are becoming increasingly tailored to individual patient needs, considering genetic predispositions and specific anatomical factors.
- Early Intervention: Greater awareness of the link between sleep apnea and facial development is driving earlier diagnosis and intervention, maximizing the potential for positive outcomes.
The Risks of Ignoring the Signs
Untreated pediatric sleep apnea can have far-reaching consequences. Chronic oxygen deprivation can impair brain development, leading to daytime sleepiness, concentration problems, learning difficulties, and behavioral issues. Long-term risks include hypertension, heart disease, and metabolic disorders. Prompt diagnosis and treatment are essential to correct facial development and improve overall health.
FAQ
Q: What are the first signs of sleep apnea in a child?
A: Loud snoring, pauses in breathing during sleep, mouth breathing, and nighttime bedwetting are common indicators.
Q: Is sleep apnea always treated with surgery?
A: No, treatment options vary depending on the severity of the condition and may include watchful waiting, orthodontics, or myofunctional therapy.
Q: How can I locate a sleep apnea specialist?
A: You can search for board-certified ENT specialists like Jacqueline Jones, M.D. At Park Avenue ENT, or consult with your pediatrician for a referral.
Did you know? Untreated sleep apnea can negatively impact a child’s academic performance and social-emotional development.
Pro Tip: If you suspect your child has sleep apnea, record a video of them sleeping to share with your doctor.
If you’re concerned about your child’s sleep, don’t hesitate to seek professional guidance. Early intervention can make a significant difference in their health and well-being. Learn more about sleep apnea treatment options.