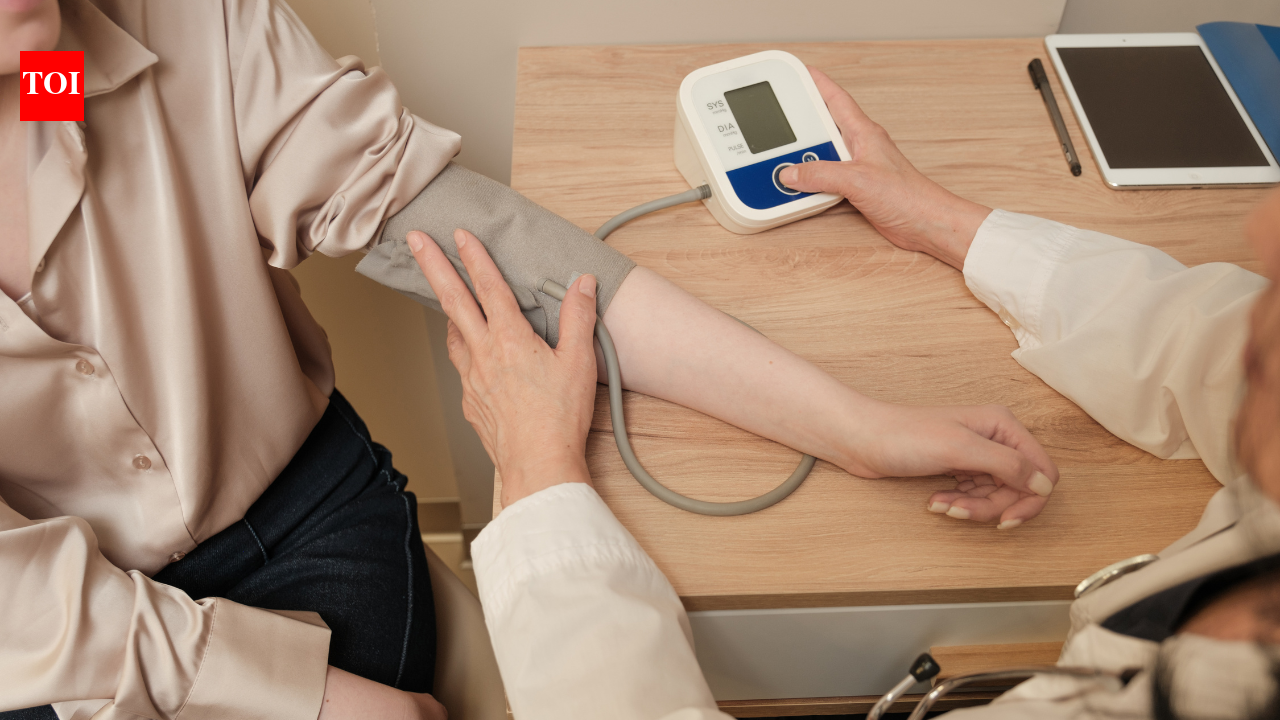
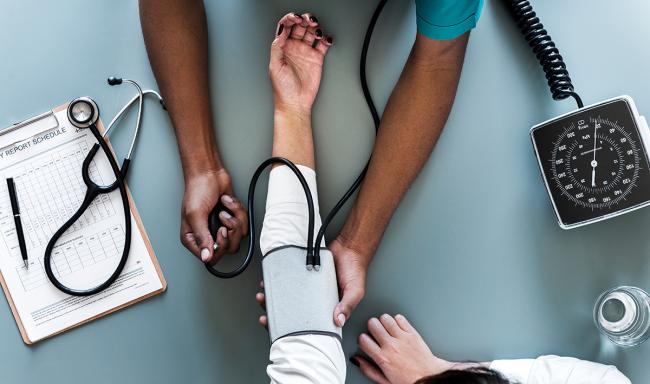
The Rise of Plant-Based Cardiology: Is Peppermint the Next Frontier in Blood Pressure Management?
For decades, the approach to managing hypertension has been relatively linear: lifestyle changes first, followed by a cocktail of pharmaceuticals. However, a shifting paradigm in integrative medicine is beginning to prioritize “nutraceuticals”—food-derived compounds with pharmaceutical-like effects. Recent evidence suggests that something as simple as peppermint oil might play a significant role in this evolution.
A groundbreaking study from the University of Lancashire, published in PLOS One, revealed that adults with mild hypertension saw their systolic blood pressure drop by an average of 8.5 mmHg after taking a small daily dose of peppermint oil for just 20 days. This isn’t just a marginal gain; in the world of cardiovascular health, a drop of this magnitude can significantly lower the risk of stroke and heart disease.
From Aromatherapy to Clinical Intervention
Peppermint oil has long been relegated to the realm of aromatherapy or digestive aids. However, the science is now catching up to the tradition. The secret lies in the oil’s rich concentration of menthol and flavonoids. These natural compounds are believed to interact with the body’s physiological parameters to induce a calming effect on the vascular system.

This trend reflects a broader movement toward evidence-based naturalism. We are seeing a transition where “natural” no longer means “unproven.” With clinical trials now exploring peppermint oil for mild-to-moderate hypertension (such as those tracked via ClinicalTrials.gov), the medical community is beginning to validate plant-based extracts as viable adjunct therapies.
The goal isn’t necessarily to replace gold-standard medications but to provide an affordable, low-side-effect alternative for those in the “prehypertension” or “stage 1” categories—people who are at risk but may not yet require heavy pharmaceutical intervention.
Future Trend: The Democratization of Heart Health
One of the most compelling aspects of using plant-based extracts like peppermint oil is the cost. As global healthcare costs skyrocket, the search for “low-cost, high-impact” interventions has become a priority for global health organizations.

Imagine a future where cardiovascular screening in developing regions is paired with accessible, plant-based supplements. Because peppermint oil is inexpensive to produce and easy to distribute, it represents a scalable solution to combat arterial hypertension—the single greatest risk factor for global mortality.
We are likely moving toward a “Hybrid Care Model” where physicians prescribe a combination of:
- Precision pharmaceuticals for high-risk patients.
- Standardized nutraceuticals (like peppermint oil) for early-stage management.
- AI-driven lifestyle tracking to monitor real-time responses to these treatments.
The Synergy of “Food as Medicine”
The success of peppermint oil is a catalyst for a larger trend: the synergy of diet and medicine. We are seeing a surge in research into other botanical extracts that target the renin-angiotensin-aldosterone system (RAAS), which regulates blood pressure and fluid balance.

Future trends suggest we will see “personalized nutrition” plans where your genetic profile determines which plant extract—be it peppermint, garlic, or omega-3s—will be most effective for your specific vascular architecture. This moves us away from the “one size fits all” pharmacy model and toward a tailored, biological approach to wellness.
For more insights into how nature is shaping modern medicine, check out our guide on the future of integrative wellness.
Frequently Asked Questions
Can peppermint oil completely replace blood pressure medication?
No. While research shows it is effective for mild hypertension or prehypertension, it is intended as a complementary or early-stage intervention. Always follow your doctor’s prescription for severe hypertension.
How is peppermint oil administered for blood pressure?
In the University of Lancashire study, participants took 100 microliters of peppermint oil orally, twice a day. It is important to use food-grade, standardized extracts rather than industrial essential oils.
What are the main active ingredients in peppermint oil?
The primary active compounds are menthol and various flavonoids, which contribute to its physiological effects on the heart rate and blood pressure.
Join the Conversation: Do you believe natural supplements will eventually replace traditional prescriptions for mild conditions? Have you tried integrative approaches to heart health? Share your thoughts in the comments below or subscribe to our newsletter for the latest breakthroughs in science and health!