The Quiet Health Crisis: Why Routine Screening is the Future of Preventative Care
Millions of Americans are navigating life unaware of underlying health conditions. It’s not that these conditions are hidden, but rather that many haven’t had a reason to look for them. The growing evidence suggests that proactive health screening isn’t just beneficial – it’s becoming essential for long-term wellbeing.
The “Feeling Fine” Fallacy
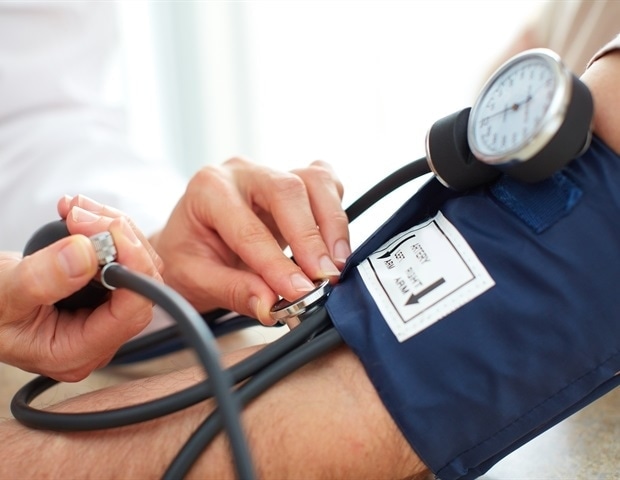
A 2025 survey revealed that nine in ten Americans have delayed or avoided health screenings, primarily because they feel healthy. This is a dangerous misconception. Conditions like type 2 diabetes, high blood pressure, and kidney disease often develop without noticeable symptoms in their early stages. By the time symptoms appear, the condition may have progressed for years.
The Power of Early Detection: What the Data Shows
A large population health study published in the American Journal of Managed Care demonstrated the impact of annual screenings. Analyzing data from over 35,000 employees, researchers identified 1,185 previously undiagnosed cases of prediabetes, 287 cases of diabetes, and 73 cases of chronic kidney disease. Early identification and care could potentially prevent 210 cases of type 2 diabetes and delay 34 cases of end-stage kidney disease per 1,000 people screened. A separate study linked a three-year delay in diagnosis to a 40 percent higher risk of cardiovascular disease.
The Economic and Human Cost of Delay
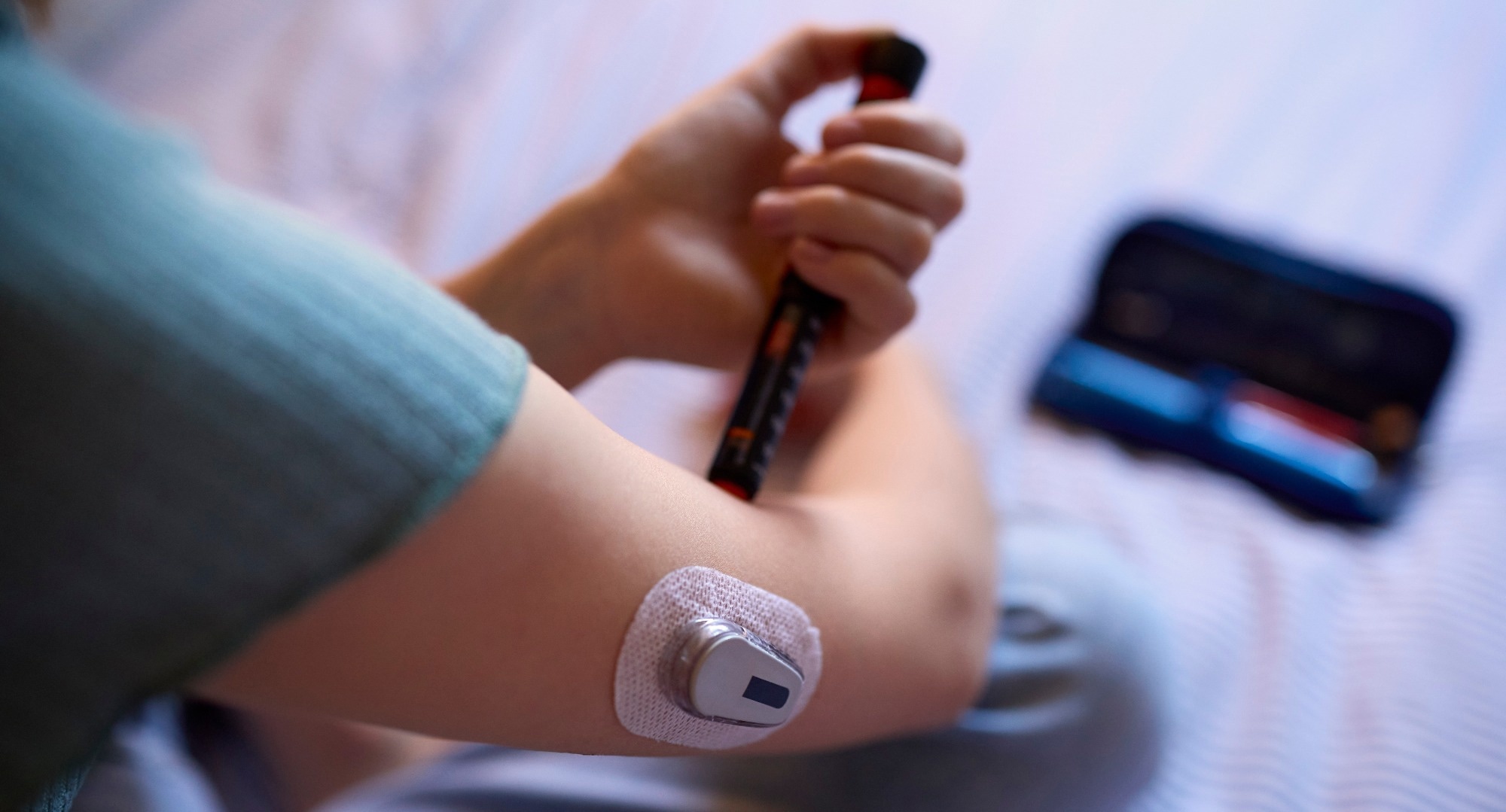
Treating conditions in their late stages is significantly more expensive – both financially and in terms of human suffering – than early intervention. The Agency for Healthcare Research and Quality estimates that preventative screening can reduce long-term healthcare costs by 20 to 30 percent per patient. Currently, over 48 percent of American adults are at risk for cardiovascular disease, much of which is detectable through routine lab panels. Nearly one in five adults with diabetes remains undiagnosed, but is manageable with early detection.
What Does Routine Lab Work Actually Reveal?
Standard blood work ordered during an annual physical typically assesses blood glucose levels, kidney and liver function, cholesterol, thyroid activity, and markers of inflammation or infection. These tests don’t require pre-existing symptoms to be ordered and can reveal hidden problems. For individuals over 50, the US Preventive Services Task Force recommends additional screening protocols, including colorectal cancer screening and bone density assessments.
Overcoming Barriers to Preventative Care
Several obstacles prevent people from getting screened, including cost, inconvenience, fear of receiving bad news, and a lack of a primary care provider. Having a regular doctor significantly increases the likelihood of staying current on screenings. For those facing financial constraints, community health centers and federally qualified health centers offer low-cost preventative screenings to eligible adults. If fear is a barrier, remember that early detection provides options, while delayed diagnosis often limits them.
The Future of Personalized Screening
The trend is moving towards more personalized and comprehensive micronutrient testing. While traditional blood panels offer a baseline assessment, emerging technologies are allowing for a deeper dive into individual nutritional status. Panels are becoming available that assess levels of vitamin D, vitamin B12, folate, magnesium, iodine, and zinc. Quest Diagnostics offers micronutrient test panels focused on antioxidants and B-vitamins, recognizing the impact of these nutrients on chronic disease prevention and overall health. These tests can help identify deficiencies that might be missed by standard assessments.
Navigating the World of Vitamin and Mineral Deficiency Tests
Labcorp’s micronutrient test measures six essential nutrients: vitamin D, vitamin B12, folate, magnesium, iodine, and zinc. Understanding your levels can empower you to make informed decisions about your diet and lifestyle. The availability of comprehensive panels from companies like UltraLabTests brings together key markers to assess energy levels, immunity, brain function, bone health, and heart health.
Frequently Asked Questions
How often should I get a vitamin panel?
The frequency depends on your age, health status, and risk factors. Discuss with your doctor to determine the best schedule for you.
What if my test results are abnormal?
Abnormal results don’t necessarily mean you have a serious condition. Your doctor will interpret the results in the context of your overall health and recommend appropriate follow-up steps.
Are micronutrient tests covered by insurance?
Coverage varies depending on your insurance plan. Check with your provider to determine if your test is covered.
A lab test isn’t a diagnosis; it’s information. In medicine, early information is almost always more valuable than the same information gathered during a crisis. If you’ve been postponing your annual checkup, remember that feeling well isn’t the same as being well. Schedule your appointment today.
Explore More: Read our article on understanding your bloodwork