The Invisible Threat: Why Lung Cancer is Rising in Non-Smokers and What the Future Holds
For decades, the medical narrative around lung cancer was simple: if you didn’t smoke, you were largely safe. But a troubling epidemiological shift is rewriting that script, particularly across Southern India. We are now seeing a surge of patients—many of them women who have never touched a cigarette—diagnosed with aggressive lung malignancies.
In cities like Hyderabad, the situation has reached a critical tipping point. With an Age-Standardized Incidence Rate (ASIR) of 6.8 per 100,000 women, the region is witnessing a health crisis that isn’t driven by lifestyle choices, but by the very air we breathe and the DNA we inherit.
The Genetic Blueprint: A Regional Vulnerability
One of the most groundbreaking revelations in recent genomic studies, specifically those conducted at the Basavatarakam Indo-American Cancer Hospital, is the discovery of a distinct genetic susceptibility among populations in Telangana and Andhra Pradesh.
certain genetic variations in these regions impair the body’s natural ability to detoxify environmental pollutants. While a person in another part of the world might be able to process and expel toxins from biomass smoke or smog, individuals with these specific markers are more prone to cellular DNA damage.
This means that for many women in South India, the “threshold” for cancer is lower. Environmental triggers that might be harmful to anyone become potentially lethal for those with this genetic predisposition.
Urbanization and the PM 2.5 Trap
The rise of adenocarcinoma—a subtype of lung cancer that develops in the peripheral lung tissues—is closely linked to ambient air pollution. In Hyderabad, the air quality has become a silent carcinogen.

Current data shows that PM 2.5 concentrations in the city have soared to 88 µg/m³, which is over 17 times the safe limit recommended by the World Health Organization (WHO). These microscopic particles are small enough to penetrate deep into the alveolar sacs, triggering chronic inflammation and mutations.
High-traffic corridors and industrial hubs like Gachibowli, Madhapur, and Patancheru have become hotspots. Pulmonologists are now reporting a phenomenon where lifelong non-smokers present with lungs showing heavy, black carbon deposits—a condition previously seen almost exclusively in heavy smokers.
Future Trends: How the Medical Landscape Will Shift
As we move forward, the approach to lung health will have to evolve from “tobacco-centric” to “environment-centric.” Here are the key trends we expect to see:
1. Precision Screening for Non-Smokers
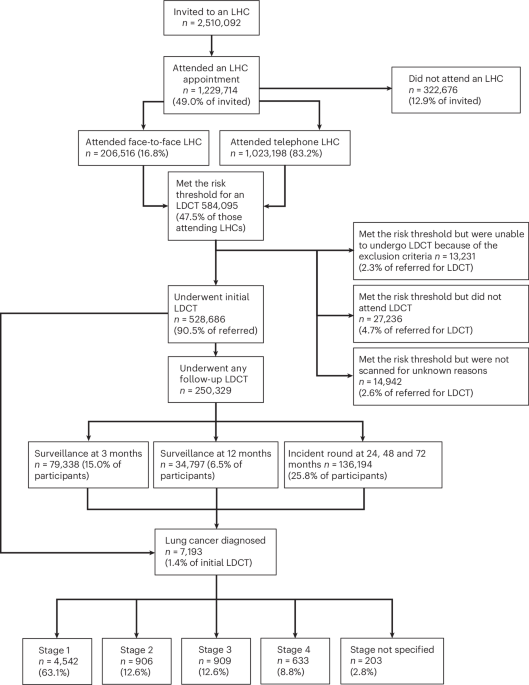
Currently, most lung cancer screenings target heavy smokers. In the future, we will likely see the implementation of risk-based screening. This will involve combining genetic testing (to identify detoxification deficiencies) with environmental exposure mapping to identify high-risk women, even if they have never smoked.
2. The Push for “Clean Kitchen” Initiatives
While urban smog is a major driver, household air pollution from biomass fuels remains a silent killer in rural areas. We anticipate a massive shift toward electrified cooking and cleaner energy sources as a direct public health intervention to lower cancer rates among rural women.

3. Integration of Environmental Data into Clinical Diagnosis
Doctors will no longer just ask, “Do you smoke?” They will ask, “Where do you live, and where did you work for the last twenty years?” Integrating geospatial pollution data into patient records will become standard for early detection of adenocarcinoma.
For more information on respiratory health, you can explore the Cleveland Clinic’s guide to lung anatomy and function to understand how pollutants affect your air sacs.
Frequently Asked Questions
Q: Can air pollution really cause cancer in someone who has never smoked?
A: Yes. Fine particulate matter (PM 2.5) is classified as a Group 1 human carcinogen. These particles cause chronic inflammation and direct DNA damage in lung cells, which can lead to malignancy over time.
Q: Why are women more affected in Southern India?
A: It is a combination of factors: prolonged exposure to domestic biomass smoke in kitchens, a specific regional genetic susceptibility to pollutants, and the impact of rapid urbanization in metro cities.
Q: What is Adenocarcinoma?
A: It is a type of lung cancer that starts in the glandular cells that secrete mucus. Unlike other types, it is frequently found in non-smokers and tends to develop in the outer edges of the lungs.
Q: Are there any early warning signs for non-smokers?
A: While early stages are often asymptomatic, a persistent cough, shortness of breath, or unexplained chest pain should be evaluated by a professional, regardless of smoking history.
Join the Conversation: Do you live in a high-pollution area, or have you noticed changes in the air quality of your city? Share your thoughts in the comments below or subscribe to our newsletter for the latest updates on public health and environmental wellness in India.