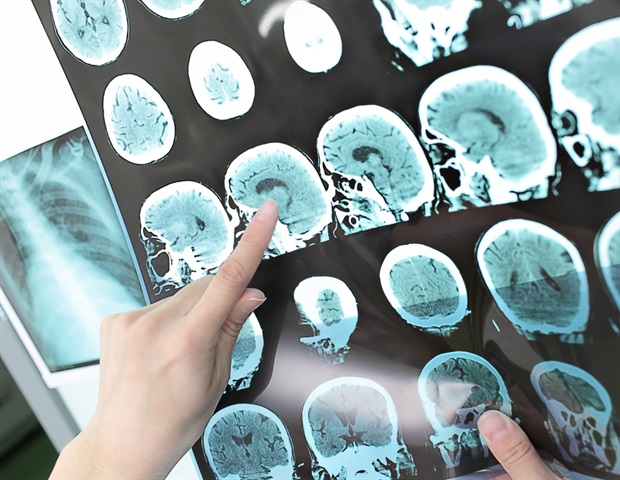
For decades, neuroscientists have been staring at a wall of overwhelming complexity. The human brain, with its roughly 86 billion neurons, has long been considered the most complicated structure in the known universe. Every attempt to map it feels like trying to count every grain of sand on a beach while a storm is blowing.
However, a paradigm shift is brewing. Recent breakthroughs in neural circuit mapping—specifically research coming out of the University of Michigan—suggest that we might not need to study every single grain of sand to understand how the beach works. Instead, we need to understand the patterns that shape them.
The End of the “One Neuron at a Time” Era
Traditionally, neuroscience has operated on a granular level, attempting to categorize and understand thousands of individual neuron types. While this meticulous approach has yielded results, it has also slowed progress. The sheer volume of data makes it nearly impossible to see the “big picture” of how behavior emerges from biology.
A groundbreaking study involving Drosophila (fruit flies) has provided a roadmap out of this complexity. By identifying that 8,000 different neurons can actually be categorized into roughly 200 “ground plans,” researchers have discovered a modular way to view the brain. This isn’t just a mathematical shortcut. It’s a fundamental discovery of how nature organizes intelligence.
Future Trend 1: Modular Neuro-Mapping and the “Blueprint” Approach
The most immediate trend following this discovery is the move toward modular neuroscience. Rather than mapping individual cells, future research will likely focus on these “ground plans”—the structural templates that dictate how circuits are formed.
We are moving toward a world where we define the brain by its architectural modules. If we understand the “ground plan” for a specific behavior—such as the “taste and cease” mechanism discovered in the Michigan study—we can predict how changes in specific regulatory genes will alter entire behavioral patterns.
Accelerated Drug Discovery
This modularity will revolutionize pharmacology. Currently, many psychiatric drugs are “blunt instruments,” affecting large areas of the brain and causing widespread side effects. By understanding the specific gene sets that create functional modules, scientists could develop precision neuro-therapeutics that target only the specific circuit responsible for a disorder, leaving the rest of the brain untouched.
Future Trend 2: The Convergence of AI and Computational Neuroscience
As we move from 8,000 variables to 200, the computational load for simulating brain activity drops exponentially. This opens the door for a new era of AI-driven brain modeling.
We are seeing the rise of “Digital Twins” of neural circuits. Using the modular framework, AI researchers can build highly accurate simulations of brain functions. These simulations can be used to test how a new medication might affect a patient’s decision-making process or motor control before a single dose is ever administered in a clinical setting.
Future Trend 3: Precision Psychiatry and Behavioral Genetics
The ultimate frontier is the application of these findings to human mental health. The Michigan study highlights how two sets of genes work in tandem: one for the “gross” shape of a neuron and one for its “fine” connectivity.

In the future, we may see a shift in how we diagnose mental health conditions. Instead of relying solely on symptomatic observation, clinicians might look at the developmental programs of a patient’s neural circuits. If a patient’s “ground plan” for impulse control is genetically predisposed to certain connectivity errors, treatment can be tailored to that specific biological blueprint.
Why This Matters for the Next Decade
The transition from “cellular neuroscience” to “circuit-based neuroscience” is more than just a change in terminology. It is a shift from description to prediction. We are no longer just asking, “What does this neuron do?” We are asking, “How does this blueprint build a mind?”
As we continue to bridge the gap between the humble fruit fly and the complex human cerebrum, the “complexity wall” is finally starting to crumble. The era of the modular brain is here.
Frequently Asked Questions (FAQ)
1. How does studying fruit flies help humans?
Fruit flies share many of the same fundamental regulatory genes that control brain development in mammals, including humans. This makes them an efficient and highly accurate model for studying complex neural processes.
2. What is a “ground plan” in neuroscience?
A ground plan refers to a modular structural template of a neuron. Instead of every neuron being unique, many share a common “blueprint” that determines their basic shape and connectivity.
3. Can this research lead to cures for brain diseases?
While it is still in the early stages, the ability to identify the specific genetic modules that control behavior could lead to highly targeted treatments for neurological and psychiatric disorders.

4. What is the significance of the two sets of genes?
One set of genes establishes the basic, large-scale structure (the ground plan), while the second set fine-tunes the connections and specific characteristics. Understanding this hierarchy allows scientists to map how behavior is built from the ground up.
Stay Ahead of the Science Frontier
The world of neuroscience is evolving faster than ever. Don’t miss our deep dives into the technologies shaping the future of humanity.
Subscribe to our Newsletter | Explore More Neuro-Tech Articles
Have thoughts on the modular brain? Let us know in the comments below!