Your Apple Watch: The Future of Heart Failure Management is Here
Toronto, ON – Forget complicated procedures and endless pills. The future of managing heart failure might be strapped to your wrist. A groundbreaking study, TRUE-HF (NCT05008692), conducted at the University Health Network, is demonstrating the potential of Apple Watch data to predict declines in heart function before patients even feel sick enough to go to the hospital. This isn’t just about counting steps; researchers are diving deep into heart rate variability, sleep patterns, and subtle changes in activity levels to get a remarkably accurate picture of cardiac health.
How Does the TRUE-HF Study Perform?
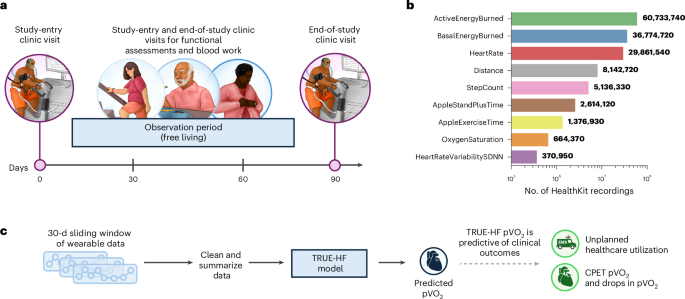
The TRUE-HF study isn’t simply handing out Apple Watches and hoping for the best. It’s a sophisticated system. Researchers collect data from the Apple Watch – including step count, exercise time, and heart rate – and feed it into a complex machine learning model. This model, developed in collaboration with Apple, analyzes the data to identify subtle changes that might indicate a worsening of heart failure. Crucially, the model focuses on trends, not just isolated data points.
Researchers have even developed methods to account for gaps in data when patients don’t wear their watch consistently, ensuring a more complete picture. The study also incorporates data from clinical tests like cardiopulmonary exercise testing (CPET) and bloodwork for a comprehensive assessment.
Predicting the Unpredictable: A Deep Dive into the Technology
The TRUE-HF model leverages a contextualized deep learning (DL) model to analyze temporal trends across 30 days of patient-wearable data. It combines wearable data with patient-specific clinical information like age, sex, and medication dosages. The model predicts an individual’s cardiopulmonary fitness and changes in that fitness over time.
A key innovation is the use of a “teacher-assistant” model when applying the TRUE-HF framework to data from different wearable devices, like Fitbits used in the All of Us Research Program. This allows the model to adapt to varying data availability and maintain accuracy.
Early Detection Saves Lives: The Impact of a 10% Drop
The study has revealed a significant correlation between a 10% drop in wearable-derived daily peak oxygen uptake (pVO2) and a 3.62-fold increased hazard ratio for unplanned healthcare events, like hospitalizations. These events occurred, on average, just 7.4 days after the initial drop in pVO2. This suggests that the Apple Watch data can provide an early warning system, allowing doctors to intervene before a crisis occurs.
External validation in the All of Us Research Program further confirmed these findings, showing a 1.32-fold increased hazard ratio for unplanned healthcare utilization with a similar drop in pVO2.
Beyond Prediction: Understanding the ‘Why’
Researchers are also using the data to understand the underlying mechanisms of heart failure exacerbations. By analyzing the interplay between various data points – heart rate variability, activity levels, sleep patterns – they hope to identify the factors that contribute to declines in heart function. This knowledge could lead to more targeted and effective treatments.
Saliency analyses are being used to quantify feature importance, helping researchers understand which data points are most predictive of adverse events.
Ethical Considerations and Data Security
The TRUE-HF study was conducted under strict ethical guidelines, with approval from the University Health Network Research Ethics Board. All participants provided informed consent, and data was collected and analyzed securely and de-identified. The wearable-derived data was not used to directly inform clinical decision-making.
Frequently Asked Questions
Q: What is pVO2 and why is it important?
A: pVO2, or peak oxygen uptake, is a measure of your body’s ability to use oxygen during exercise. A decline in pVO2 is often an early sign of worsening heart failure.
Q: Is this technology available to patients now?
A: While the TRUE-HF study is ongoing, the results are promising and could pave the way for wider adoption of wearable technology in heart failure management in the future.
Q: What kind of Apple Watch data is being used?
A: Researchers are collecting data on step count, exercise time, distance traveled, stand time, active energy burned, heart rate, heart rate variability, and oxygen saturation.
Q: How accurate is the Apple Watch data?
A: The study has shown a strong correlation between Apple Watch-derived pVO2 and CPET-measured pVO2 (Pearson’s correlation = 0.85).
Q: What about privacy concerns?
A: Data is collected securely and de-identified to protect patient privacy.
Pro Tip: Maintaining consistent Apple Watch wear is crucial for accurate data collection and reliable predictions.
Did you know? A 10% drop in wearable-derived daily pVO2 can be an early indicator of an impending heart failure event, potentially allowing for proactive intervention.
Desire to learn more about the latest advancements in heart failure research? Explore the full study details on Nature.com.
Share your thoughts on the potential of wearable technology in healthcare in the comments below!