AI’s Promise for Lung Cancer Detection: A Reality Check
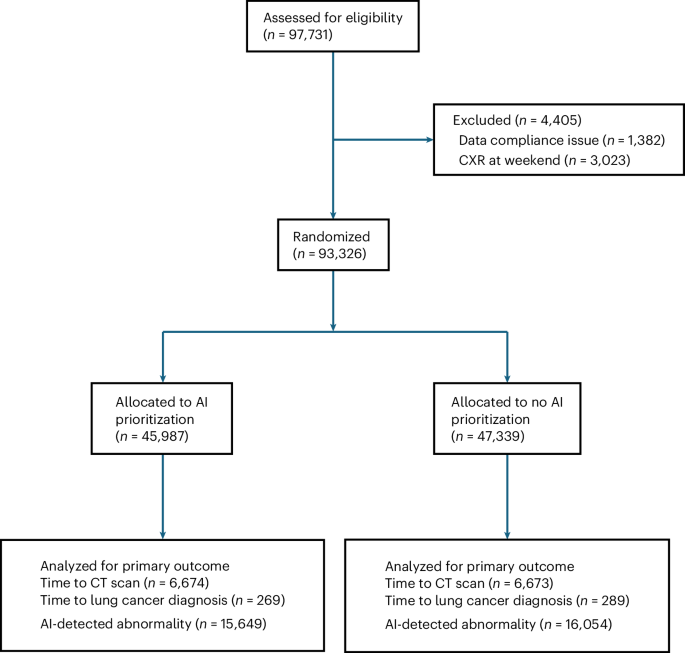
The push to leverage artificial intelligence in healthcare continues, with significant investment focused on improving early disease detection. However, a large-scale UK study, published in Nature Medicine, has delivered a sobering assessment of AI’s current capabilities in accelerating lung cancer diagnosis. The LungIMPACT trial, involving over 93,000 chest X-rays (CXRs), found that AI-driven prioritization of scans did not significantly shorten the time to crucial CT scans or final cancer diagnoses.
The Bottleneck Isn’t the Scan, It’s the System
Researchers discovered that whereas AI did reduce the time it took for a radiologist to initially review a CXR – from 47 hours to 34 hours – this speed boost didn’t translate into faster overall diagnosis. The issue, it appears, lies in the downstream processes within the National Health Service (NHS). As Dr. Nick Woznitza, the principal investigator, explained, the bottleneck isn’t the reporting; it’s scheduling patient follow-ups, CT appointments, and multidisciplinary team reviews.
This finding highlights a critical point: technology alone isn’t a panacea. Even with faster image analysis, existing systemic constraints can negate the benefits. The study underscores the need for comprehensive pathway redesign, not just technological upgrades.
Discordance and the ‘Cry Wolf’ Effect
The study also delved into instances where AI and radiologists disagreed on their interpretations of CXRs – a phenomenon known as discordance. These disagreements occurred in nearly 30% of cases (28,261 CXRs). Researchers noted the potential for “vigilance fatigue,” where radiologists might grow desensitized to subtle abnormalities or lose trust in the AI’s accuracy if it frequently flags scans that ultimately prove benign – the so-called “cry wolf” effect.
This concern is echoed by the National Institute for Health and Care Excellence (NICE), which has not yet recommended any AI products for CXR interpretation in England.
What Does This Mean for the Future of AI in Lung Cancer Screening?
Despite these findings, the potential of AI in lung cancer detection isn’t entirely dismissed. The LungIMPACT trial focused specifically on prioritization. AI’s role as a diagnostic aid – assisting radiologists in identifying subtle anomalies – remains an area of active research. Several studies suggest AI can improve detection rates, increasing sensitivity to 83.3% when used in conjunction with radiologists.
However, the current evidence suggests that simply flagging scans for faster review isn’t enough. Future strategies may need to focus on integrating AI more deeply into the clinical workflow, potentially prompting immediate radiologist review for AI-flagged abnormalities and triggering a coordinated “bundle” of investigations.
The Importance of Robust Data and Real-World Testing
The LungIMPACT trial’s strength lies in its large scale and randomized controlled design. It analyzed data from five NHS trusts, providing a realistic assessment of AI’s performance in a diverse clinical setting. The study’s focus on unselected cases – CXRs requested in primary care – further enhances its relevance.
This contrasts with some other studies, which have used retrospectively selected data or enriched datasets (focusing on cases with specific findings). The real-world applicability of these studies is often limited.
Frequently Asked Questions
- Does AI have any role in lung cancer diagnosis? Yes, AI shows promise as a diagnostic aid for radiologists, potentially improving detection rates.
- Why didn’t AI prioritization speed up diagnosis in this study? Systemic bottlenecks in the NHS, such as appointment scheduling and multidisciplinary team reviews, prevented the benefits of faster image analysis from translating into faster overall diagnosis.
- What is ‘vigilance fatigue’? It’s the potential for radiologists to become desensitized to abnormalities or lose trust in AI if it frequently flags scans that turn out to be benign.
- Is AI currently recommended for CXR interpretation in England? No, NICE has not yet recommended any AI products for this purpose.
Pro Tip: Don’t rely solely on technology. A well-coordinated clinical pathway, with efficient communication and timely follow-up, is crucial for improving lung cancer diagnosis rates.
Did you know? Over 7 million chest X-rays are performed annually in England, with approximately 2.2 million originating from primary care referrals.
Desire to learn more about the latest advancements in medical imaging and AI? Explore our other articles on digital health and precision medicine.