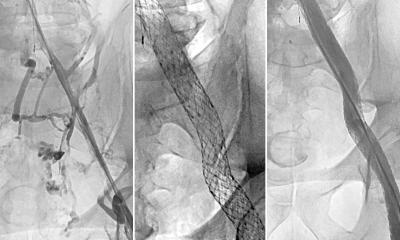
New Hope for Millions: Minimally Invasive Treatment Offers Relief from Post-Thrombotic Syndrome
For years, patients suffering from post-thrombotic syndrome (PTS) – a debilitating condition following deep vein thrombosis (DVT) – have faced limited treatment options. Now, a groundbreaking clinical trial is changing that landscape, offering a path to improved quality of life for the over 300,000 Americans diagnosed with DVT annually.
Understanding the Silent Suffering of Post-Thrombotic Syndrome
Deep vein thrombosis, often occurring in the leg, carries a significant risk of pulmonary embolism, a potentially fatal condition. Although preventing new clots is the primary focus of treatment, the damage left behind by DVT often leads to PTS. Approximately 40% of DVT survivors develop PTS, experiencing symptoms like leg pain, swelling, skin discoloration, and impaired mobility. In severe cases, chronic ulcers can form, significantly impacting daily life.
“We see a lot of patients who have moderate or severe post-thrombotic syndrome and have a tough time conducting their daily activities and maintaining a good quality of life,” explains Dr. Suresh Vedantham, lead author of the study and an interventional radiologist at Washington University School of Medicine in St. Louis. “Many patients are unable to walk without pain or work productively.”
The C-TRACT Trial: A Turning Point in PTS Treatment
The Chronic Venous Thrombosis: Relief with Adjunctive Catheter-Directed Therapy (C-TRACT) Trial, sponsored by the National Institutes of Health (NIH), investigated the effectiveness of a minimally invasive procedure: the placement of a stent to reopen blocked veins. The trial, conducted across 29 sites in the U.S., enrolled 225 patients with significant blockage in the iliac vein.
Patients were randomly assigned to receive either a stent, along with standard treatment (compression and blood thinners), or standard treatment alone. The results were compelling. Six months after treatment, only 40% of patients who received a stent still experienced severe PTS, compared to 61% in the standard care group. Patients with stents reported a 14-point improvement on a 100-point quality of life scale.
How Stenting Works: Restoring Blood Flow and Reducing Symptoms
The procedure itself is relatively quick, taking two to three hours and requiring only tiny incisions. A stent, a mesh tube, is inserted into the blocked vein to reinforce and expand it, restoring proper blood flow. This addresses the underlying cause of PTS, unlike traditional treatments like compression stockings, which primarily manage symptoms.

“Post-thrombotic syndrome can be life‑altering, yet we’ve had highly few effective treatment options,” says Dr. Sameer Parpia, senior author of the study and an associate professor at McMaster University. “This trial provides clear evidence that targeted therapy can make a meaningful difference for patients living with this condition.”
Future Trends: Personalized PTS Management and Beyond
The success of the C-TRACT trial signals a shift towards more proactive and targeted treatment of PTS. Several key trends are emerging:
- Early Intervention: Identifying and treating venous blockages soon after a DVT diagnosis may prevent the development of PTS altogether.
- Advanced Imaging: Improved imaging techniques will allow for more accurate diagnosis and assessment of venous blockages, guiding treatment decisions.
- Personalized Stent Selection: Research is underway to determine the optimal stent type and size for individual patients, maximizing effectiveness.
- Combination Therapies: Exploring the potential benefits of combining stenting with other therapies, such as targeted medications to prevent scar tissue formation.
Dr. Vedantham believes this trial will “provide a foundation for improving patient care for post-thrombotic syndrome and aid physicians to better understand options that they can recommend for their patients seeking treatment for the condition.”
FAQ
What is post-thrombotic syndrome? PTS is a long-term complication of deep vein thrombosis, causing pain, swelling, and other symptoms in the affected limb.
How is PTS currently treated? Traditional treatments include compression stockings and blood thinners, but these often provide limited relief.
What are the benefits of stenting? Stenting can reopen blocked veins, restoring blood flow and significantly improving symptoms and quality of life.
Is stenting right for everyone with PTS? The C-TRACT trial focused on patients with blockage in the iliac vein. A physician can determine if stenting is an appropriate treatment option based on individual circumstances.
Did you know? PTS affects a significant number of DVT survivors, yet it has historically been an undertreated condition.
Pro Tip: If you’ve experienced a DVT, discuss your risk of developing PTS with your doctor and explore all available treatment options.
Have you or a loved one been affected by PTS? Share your story in the comments below. Learn more about deep vein thrombosis and post-thrombotic syndrome by visiting the WashU Medicine website.