The New Frontier of Global Health: Why Zoonotic Spillovers are the Next Big Challenge
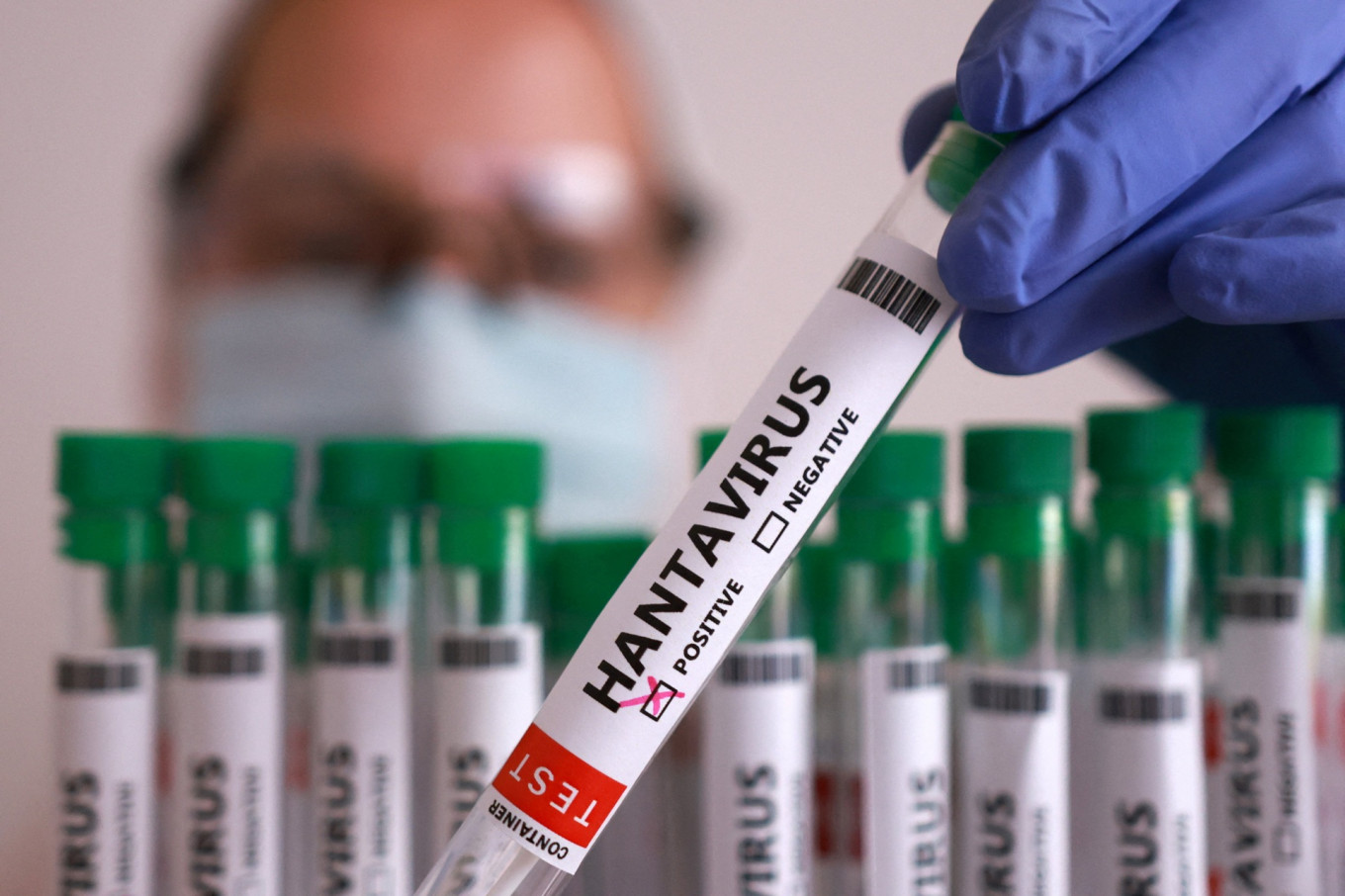
The recent alarm bells ringing over hantavirus infections on international cruise ships are more than just a localized health scare. They serve as a stark reminder of a growing vulnerability in our interconnected world: the “zoonotic spillover.”

When a virus jumps from an animal host—in this case, rodents—to humans, the results can be unpredictable. But when that jump happens in the confined environment of a luxury liner or a crowded international flight, a local incident can rapidly transform into a global surveillance operation.
The ‘Super-Vector’ Phenomenon: Travel as a Catalyst
Modern travel has created what epidemiologists call “super-vectors.” Cruise ships, with their high population density and multi-continent itineraries, are essentially floating microcosms. A passenger can be exposed to a pathogen in South America and be in a major Asian hub within 48 hours.
The case of the Andes strain of hantavirus is particularly concerning because, unlike many other hantaviruses, it has shown a capacity for limited human-to-human transmission. This shift—from animal-to-human to human-to-human—is the “red line” that health authorities watch most closely.
As global tourism rebounds and expands into more remote “adventure” destinations, the likelihood of encountering rare viral strains increases. We are moving toward an era where health screenings may become as routine as passport checks for specific high-risk corridors.
The Shift Toward Genomic Surveillance
In the past, identifying a virus took weeks of laboratory culture. Today, the trend is shifting toward real-time genomic sequencing. By mapping the genetic code of a virus the moment it is detected, scientists can determine if a strain has mutated to become more contagious.

This allows agencies like the World Health Organization (WHO) to issue targeted alerts, preventing unnecessary mass panic while ensuring that high-risk individuals are quarantined effectively.
One Health: The Integrated Approach to Future Pandemics
The future of disease prevention lies in the “One Health” approach. This strategy recognizes that human health is inextricably linked to the health of animals and the environment.
Instead of waiting for a human to show up in an ER with respiratory distress, future trends point toward environmental sentinel monitoring. This involves testing wild rodent populations in high-risk areas to predict outbreaks before they ever reach a human host.
- Urban Planning: Reducing rodent habitats in expanding cities to lower spillover risks.
- Climate Tracking: Monitoring how warming temperatures push animal carriers into new territories.
- Cross-Border Data Sharing: Instantaneous sharing of zoonotic hits between nations to trigger early warnings.
Navigating the ‘New Normal’ of Health Vigilance
For the average traveler, this doesn’t mean staying home. It means adopting a posture of “informed vigilance.” The focus is shifting from blanket lockdowns to precision public health—using data to isolate the risk without paralyzing the economy.
We are seeing a rise in digital health passports and integrated tracking systems that can alert a traveler if they have passed through a zone with an active zoonotic outbreak. While this raises privacy questions, the trade-off is a significantly faster response time to contain rare strains like the Andes virus.
Frequently Asked Questions
What exactly is a zoonotic virus?
A zoonotic virus is an infectious agent that is transmitted from animals to humans. Examples include rabies, Ebola, and various strains of influenza.
How is hantavirus typically spread?
Most hantaviruses are spread through the inhalation of aerosolized particles from the urine, droppings, or saliva of infected rodents.
Can any hantavirus spread between people?
Generally, no. However, the Andes strain (found primarily in South America) is a notable exception, as it has demonstrated the ability for limited human-to-human transmission.
What are the early warning signs of hantavirus?
Early symptoms often mimic the flu, including fever, muscle aches, and fatigue, which can quickly progress to severe respiratory distress.
Stay Ahead of the Curve
Do you think global travel should include more stringent health screenings to prevent the next spillover? We want to hear your thoughts in the comments below!
Subscribe to our Health & Global Affairs newsletter for weekly insights into the trends shaping our world.