The recently enacted 2025 reconciliation law, dubbed the “One Big Stunning Bill,” is poised to reshape Medicaid eligibility requirements for millions of Americans. Starting January 1, 2027, adults participating in the Affordable Care Act (ACA) Medicaid expansion, as well as those in partial expansion programs in states like Georgia and Wisconsin, will be required to meet work requirements to maintain their coverage.
The Looming Shift in Medicaid Eligibility
Currently, 41 states plus the District of Columbia have expanded Medicaid to cover adults earning up to 138% of the Federal Poverty Level (FPL), which was $21,597 for an individual in 2025. This expansion has been a cornerstone of increasing health insurance coverage in the U.S. The introduction of work requirements represents a significant policy shift, potentially impacting access to care for a substantial portion of the Medicaid population.
What Implementing Work Requirements Entails
States face a complex undertaking in implementing these new requirements. It’s not simply a matter of adding a new rule; it demands substantial operational changes. These include updating existing systems, developing robust outreach programs to educate beneficiaries and hiring and training staff to manage the new processes. The timeframe for these preparations is relatively short, adding to the challenge.
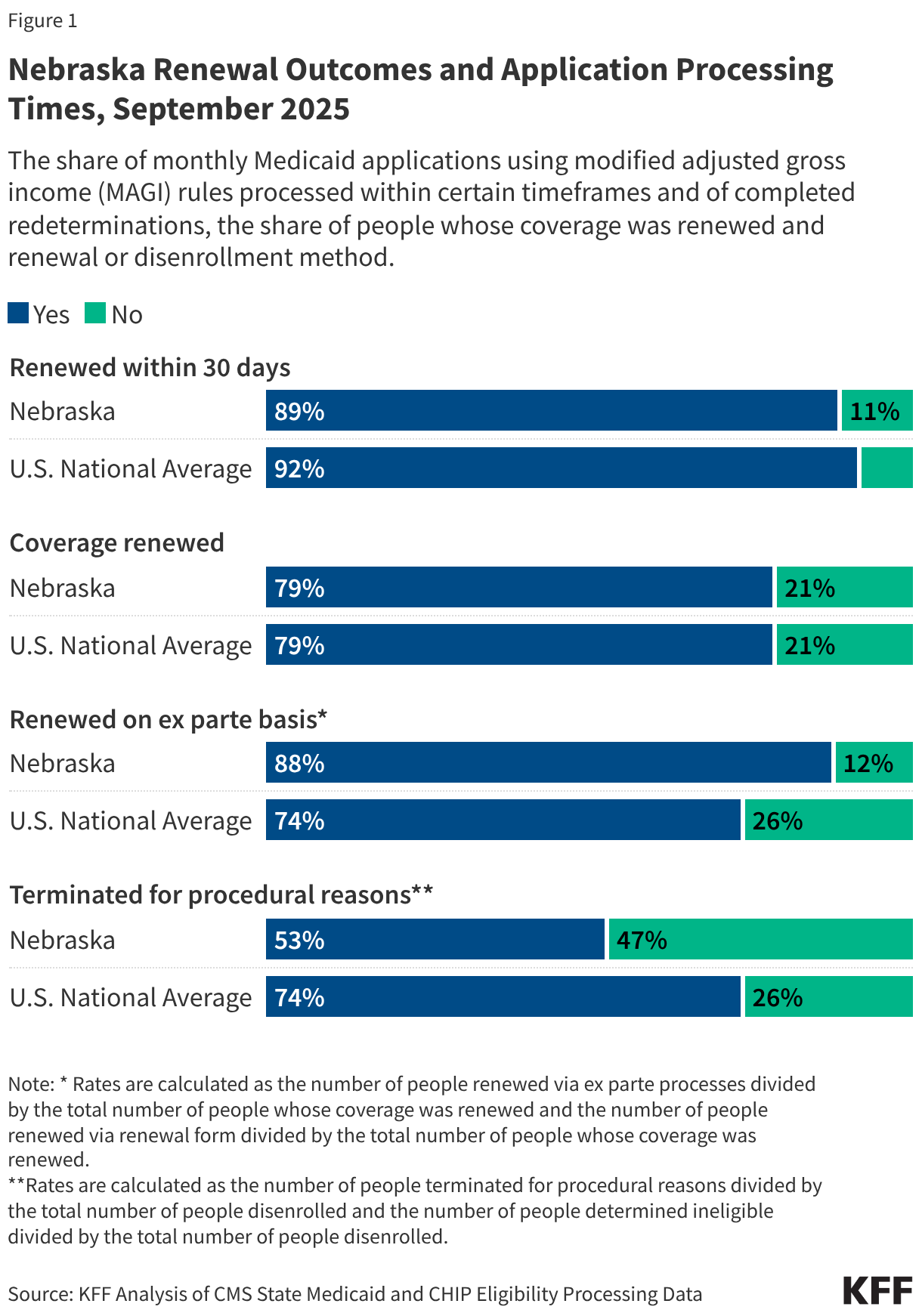
The Kaiser Family Foundation (KFF) is tracking state and national data related to Medicaid enrollment, renewal outcomes, and application processing times. This data will serve as a crucial baseline for assessing states’ readiness and the eventual impact of the work requirements.
Federal Guidance and State Waivers
While work requirements will be mandated starting in 2027, states may choose to implement them sooner through 1115 waivers. These waivers allow states to test innovative approaches within Medicaid, but they require federal approval. KFF is likewise monitoring these waiver submissions and providing updates on the process.
Potential Impacts and Ongoing Concerns
The introduction of work requirements raises concerns about potential coverage losses. Individuals facing barriers to employment – such as disability, lack of transportation, or childcare challenges – may struggle to meet the requirements and could lose their Medicaid benefits. This could lead to increased uninsurance rates and reduced access to healthcare services.
the administrative burden on states is significant. Ensuring accurate tracking of work hours, verifying employment status, and providing support to beneficiaries navigating the new system will require substantial resources.
Pro Tip: States considering early implementation through waivers should carefully analyze their existing data on beneficiary employment status and potential barriers to work to inform their waiver proposals.
Resources for Staying Informed
KFF offers a comprehensive collection of resources on Medicaid work requirements, including issue briefs, state-by-state data, and updates on federal guidance. These resources can help stakeholders understand the complexities of the new law and its potential implications.
FAQ
- When do Medicaid work requirements head into effect? Work requirements will be implemented starting January 1, 2027.
- Which states are affected? States that have expanded Medicaid under the ACA, as well as Georgia and Wisconsin with partial expansion programs, are affected.
- Where can I find more information? The Kaiser Family Foundation (https://www.kff.org/medicaid/medicaid-work-requirements-tracker/) provides comprehensive resources.
The changes to Medicaid eligibility represent a significant shift in healthcare policy. Ongoing monitoring of state implementation efforts and data on coverage rates will be crucial to understanding the full impact of these new requirements.
What are your thoughts on the new Medicaid work requirements? Share your perspective in the comments below!