Measuring the size of a brain tumor has long been a primary way to track glioblastoma, but volume alone rarely tells the whole story. A research team from the Universitat Politècnica de València (UPV) has developed a new biomarker that looks past the dimensions of a tumor to analyze how it actually interacts with the surrounding brain, offering a more precise way to assess aggressiveness and predict patient survival.
Moving beyond tumor volume
Glioblastoma is among the most aggressive forms of brain cancer, characterized by its ability to infiltrate healthy brain tissue. For clinicians, the challenge has been that traditional imaging often focuses on gross volumetric increases—how much the tumor has grown—or the displacement of brain structures. These metrics can miss the subtle, “stealthy” ways a tumor expands into the brain without causing obvious compression.

Researchers at the Biomedical Data Science Laboratory (BDSLab) within the ITACA Institute of the UPV, in collaboration with Oslo University Hospital, have introduced the Dynamic Infiltration Rate (DIR) to fill this gap. Published in the journal Medical Physics, the study presents a method that combines volumetric growth over time with the mechanical effects that growth exerts on adjacent tissue.
The mechanics of infiltration
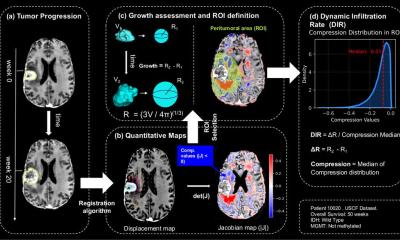
The DIR biomarker relies on longitudinal analysis of magnetic resonance imaging (MRI). By generating tissue compression maps, the team can objectively quantify whether a tumor is simply pushing against the brain or actively infiltrating it.
This distinction is critical for understanding biological behavior. The researchers found that DIR allows them to differentiate between two distinct patterns:
- Proliferative tumors: These typically grow in a way that compresses the surrounding brain structures.
- Infiltrative tumors: These expand more subtly, infiltrating healthy tissue without causing significant mechanical compression.
“Until now, assessment methods have mainly been based on measuring the increase in tumour size or the displacement of brain structures, without adequately capturing how the tumour grows or its biomechanical impact on the surrounding brain,” explains Carles López Mateu, the study’s lead author.
By integrating these biomechanical markers, the DIR provides a more comprehensive view of a tumor’s aggressiveness than size alone, which the team notes can independently predict patient survival.
Research Context: The Challenge of Infiltration
Glioblastomas are notoriously difficult to treat because they do not have clear borders. Their tendency to send microscopic “tentacles” of cancer cells into healthy brain tissue means that even if the main tumor mass is surgically removed, infiltrative cells often remain, leading to recurrence.
Implications for neuro-oncology
The ability to characterize a tumor’s behavior beyond its size could lead to more personalized treatment strategies. If clinicians can identify an infiltrative pattern early through DIR, it may change how they approach the aggressiveness of the intervention or the monitoring of the patient.
The study was a collaborative effort involving Carles López Mateu, María Gómez Mahiques, F. Javier Gil Terrón, Víctor Montosa i Micó, Juan M. García-Gómez, and Elies Fuster García. Their work suggests that the fusion of spatial-temporal growth patterns and mechanical tissue deformation creates a more intricate and useful map of tumor behavior than previously available.
Clinical Q&A
How does DIR differ from a standard MRI scan?
A standard MRI provides a snapshot of the tumor’s size and location. DIR uses longitudinal MRI data (scans over time) to create compression maps, analyzing the mechanical pressure and infiltration patterns the tumor exerts on the surrounding brain.
Does this biomarker provide a cure for glioblastoma?
No. DIR is a diagnostic and prognostic tool. It helps clinicians better understand the aggressiveness of the tumor and predict survival, which can inform treatment planning, but it is not a treatment itself.
As these biomechanical mapping techniques move toward broader clinical use, how might the ability to predict tumor infiltration change the way surgeons plan brain resections?