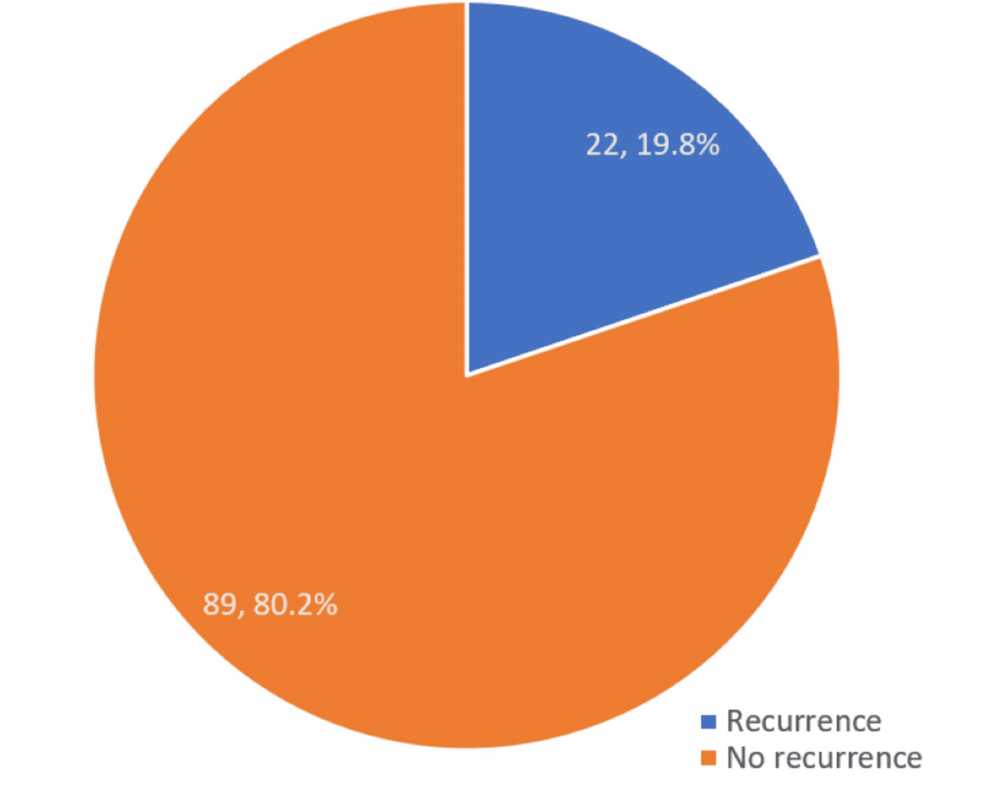
The pursuit of predictable, long-term success in treating apical prolapse remains a central challenge in urogynecological surgery. A recent prospective cohort study published in Cureus has focused on the recurrence rates and specific risk factors associated with Sacrospinous Ligament Fixation (SSLF), a surgical intervention designed to provide critical support to the top of the vagina. Understanding why some patients experience a return of prolapse while others do not is essential for improving patient selection and surgical precision.
The objective of Sacrospinous Ligament Fixation
Apical prolapse occurs when the apex—the highest point of the vaginal vault—loses its support, often leading to the descent of the uterus or the vaginal top. Sacrospinous Ligament Fixation (SSLF) is a surgical technique intended to correct this by anchoring the vaginal apex to the sacrospinous ligament, a strong structure in the pelvic basin.
While the procedure is a recognized standard for restoring anatomy, the primary concern for both surgeons and patients is recurrence. By tracking outcomes in a prospective cohort, researchers aim to move beyond anecdotal success and identify the precise clinical markers that increase the likelihood of the prolapse returning.
Clinical Context: Apical Prolapse
Apical prolapse refers specifically to the descent of the vaginal apex. This is distinct from anterior or posterior prolapse (which involve the bladder or rectum) and often requires specialized fixation techniques to ensure the vaginal vault remains stable and supported.
Identifying the drivers of recurrence
The value of a prospective study lies in its ability to follow patients forward in time, allowing clinicians to see exactly when and why a repair might fail. Identifying risk factors—such as patient age, comorbidities, or the severity of the initial prolapse—allows for a more personalized approach to treatment.

When surgeons can identify high-risk candidates, they can better manage expectations or consider alternative or adjunctive strategies to reinforce the repair. This shift toward risk-stratification is a key part of modern evidence-based medicine, ensuring that the surgical plan matches the patient’s specific anatomical and physiological needs.
The broader landscape of prolapse management
The focus on SSLF recurrence is part of a larger, global effort to refine how pelvic organ prolapse (POP) is managed. The diversity of treatment approaches is evident in recent medical literature:
- Surgical Variations: While some patients undergo ligament fixation, others are treated with mesh. For instance, research has looked into the long-term outcomes of Restorelle® Direct Fix Anterior Mesh to evaluate its efficacy in treating prolapse.
- Global Health Disparities: The management of POP varies significantly by region and available resources. A retrospective review of a tertiary referral hospital in Southwestern Uganda (2014–2018) highlighted the magnitude and presentation of prolapse in different populations, emphasizing that management strategies must be adaptable to the healthcare infrastructure available.
These varied data points suggest that there is no one-size-fits-all solution for POP. Whether using ligament fixation or mesh, the goal remains the same: reducing the rate of recurrence and improving the quality of life for the patient.
Analyzing surgical outcomes
Does a high recurrence rate indicate the surgery failed?
Not necessarily. Recurrence is a known risk in pelvic floor surgery. The goal of research into risk factors is not to eliminate the procedure, but to refine who receives it and how it is performed to maximize the chance of a permanent fix.
How do risk factors influence the decision to operate?
If a patient presents with multiple risk factors identified in prospective studies, a surgeon might opt for a more robust fixation method or implement stricter post-operative activity restrictions to protect the surgical site during healing.
How should the balance between surgical intervention and conservative management be weighed when the risk of recurrence is high?