Beyond the Clinic: The Dawn of Proactive Pediatric Respiratory Care
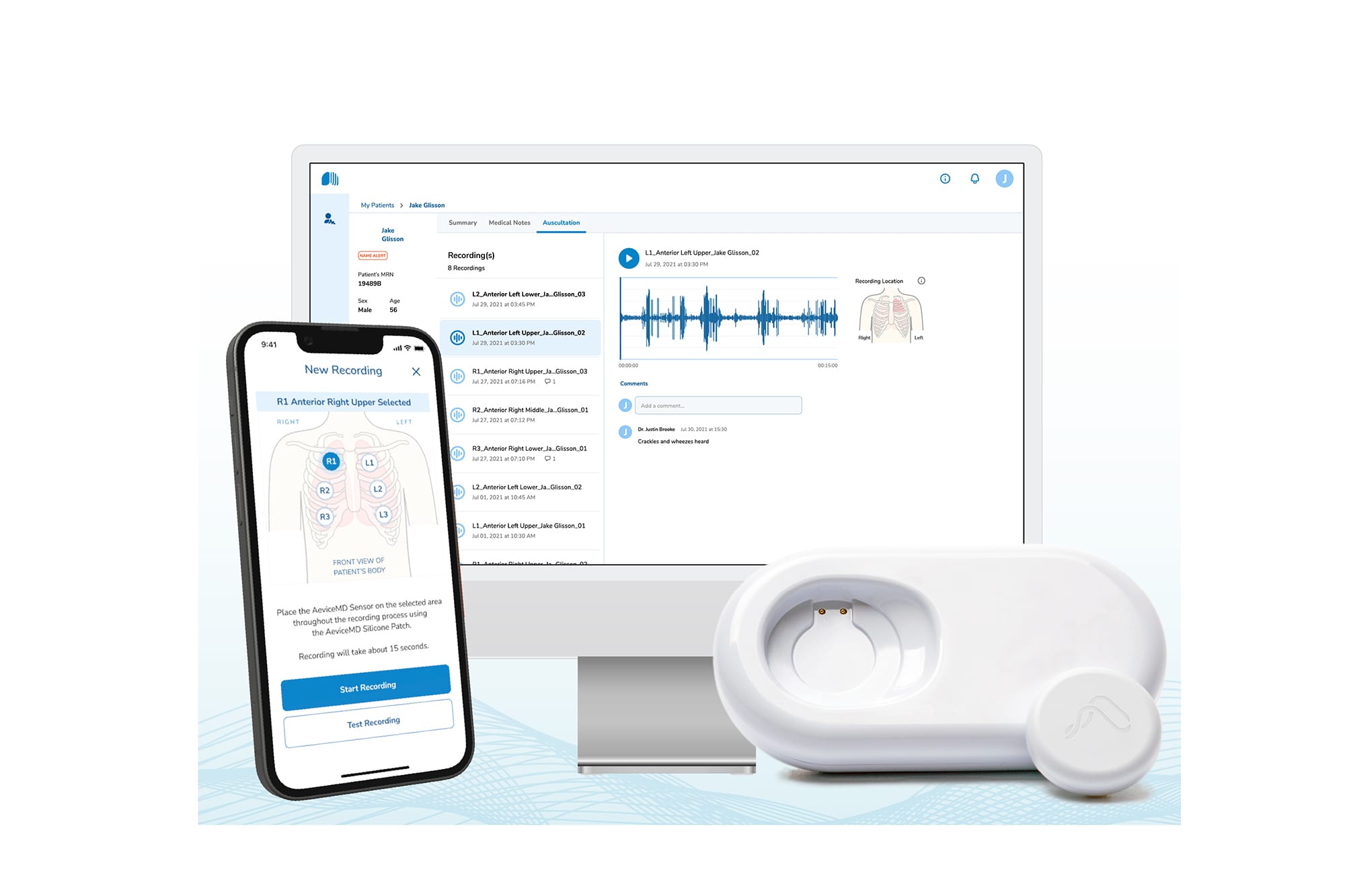
For decades, managing pediatric asthma has been a game of catch-up. Parents monitor for rapid breathing or chest congestion, and doctors rely on “snapshot” data from occasional clinic visits. But the landscape is shifting. The deployment of technologies like the AeviceMD wearable stethoscope at Cedars-Sinai Guerin Children’s marks a pivotal transition from reactive treatment to proactive management.

When we can track lung sounds in real-time—especially during the vulnerable overnight hours—we stop guessing and start knowing. This isn’t just about a new gadget; it’s about a fundamental redesign of the patient-provider relationship.
The Rise of the ‘Hospital at Home’ Model
The integration of wearable stethoscopes is a harbinger of a larger trend: the “Hospital at Home” movement. By moving diagnostic tools out of the sterile environment of a hospital and into the living room, healthcare providers are reducing the burden on emergency departments.
Imagine a future where a child’s wearable device detects a subtle change in wheezing patterns and automatically alerts a pediatric pulmonologist. Instead of a midnight trip to the ER, the parent receives a notification to adjust medication or schedule a virtual check-in. This seamless loop reduces the reliance on systemic steroids, which often carry significant side effects for growing children.
This shift is supported by the broader growth of Remote Patient Monitoring (RPM), which is transforming chronic disease management across all age groups.
Precision Pediatrics: Tailoring Treatment to Real-Time Data
We are moving toward an era of “Precision Pediatrics.” Rather than applying a one-size-fits-all asthma action plan, clinicians can now use longitudinal data to see exactly how a specific child responds to a particular medication.
By analyzing lung sounds over days and weeks, doctors can build a “respiratory fingerprint” for each patient. This allows for hyper-personalized treatment plans that evolve in real-time, ensuring that medication is scaled up or down based on physiological evidence rather than symptomatic guesswork.
AI and the Future of Acoustic Diagnostics
The current generation of wearables allows clinicians to listen to recordings, but the next frontier is Artificial Intelligence (AI). We are heading toward a world where AI algorithms can analyze thousands of hours of lung sounds to detect patterns invisible to the human ear.
Future iterations of these devices will likely feature predictive analytics. Instead of alerting a doctor that a child is having a flare-up, the AI will predict that a flare-up is likely to occur within the next 48 hours based on subtle acoustic shifts. This “predictive window” is where the most significant lives will be saved and hospitalizations avoided.
This trend mirrors the evolution of digital health innovation seen in cardiology, where AI-driven ECGs now predict cardiac events before they happen.
Global Collaboration as a Catalyst for Innovation
The partnership between Aevice Health (a Singaporean firm) and Cedars-Sinai highlights a critical trend: the globalization of MedTech. Innovation is no longer siloed within a single country’s borders. When cutting-edge engineering from Asia meets the clinical rigor of world-class US healthcare systems, the pace of FDA clearance and deployment accelerates.
This cross-border synergy ensures that pediatric patients benefit from the best global research, leading to devices that are smaller, more durable, and more accurate—such as the current coin-sized wearables that children can wear comfortably for hours.
Frequently Asked Questions
How does a wearable stethoscope differ from a traditional one?
Traditional stethoscopes provide a momentary snapshot during a clinic visit. Wearables provide continuous or on-demand monitoring in the patient’s natural environment, capturing symptoms that might not be present during a scheduled appointment.

Is this technology safe for particularly young children?
Current devices, like the AeviceMD, are specifically designed for children aged 3 and older, ensuring the fit and materials are safe for pediatric skin and activity levels.
Will remote monitoring replace doctor visits?
No. Remote monitoring is designed to supplement clinical care. It provides doctors with better data to make informed decisions during visits and allows for urgent interventions between appointments.
Join the Conversation on Health Tech
Do you believe wearable diagnostics will become the standard of care for all chronic childhood illnesses? We want to hear your thoughts!
Leave a comment below or subscribe to our newsletter for the latest insights into the future of medicine.