Beyond the Outbreak: The Future of Campus Health and Meningitis Prevention
Recent clusters of meningococcal disease in student populations—most notably in areas like Reading and Kent—serve as a stark reminder that rare diseases can still strike with sudden intensity. While these incidents are often contained quickly, they signal a broader need to evolve how we protect young adults in high-density living environments.
The challenge isn’t just the bacteria itself, but the unique social architecture of college life. Close-contact living, shared dining, and intense social circles create the perfect storm for rapid transmission. As we look toward the future of public health, the focus is shifting from reactive containment to proactive, precision prevention.
The Shift Toward Precision Epidemiology
One of the most critical takeaways from recent outbreaks is the role of strain identification. Experts have noted that different clusters, such as those in Kent and Reading, can be caused by distinct strains of the bacteria. Which means a “one size fits all” approach to vaccination may no longer be sufficient.
The future of outbreak management lies in genomic surveillance. By sequencing the DNA of the bacteria in real-time, health officials can determine exactly which strain is circulating and deploy the specific vaccine or antibiotic treatment most likely to work.
This precision approach reduces the need for mass prophylaxis—where everyone in a community is treated—and allows for targeted intervention, minimizing side effects and reducing the strain on healthcare infrastructure.
Digital Contact Tracing: The Next Frontier
Traditional contact tracing relies on memory and interviews, which can be slow. We are moving toward a future where digital footprints and integrated health apps could alert “at-risk” individuals within minutes of a confirmed case.

Imagine a system where a student tests positive, and an automated, secure notification is sent to everyone they have been in close proximity with over the last 48 hours, directing them to the nearest clinic for preventative antibiotics. This would transform the “window of vulnerability” from days to hours.
Reimagining Vaccine Strategies for Young Adults
For too long, meningitis vaccinations have been viewed as a childhood requirement. However, the “college-age cohort” remains a high-risk group due to changes in immunity and increased exposure.
Future trends suggest a move toward booster-centric models. Rather than a single series of shots in infancy, public health experts are advocating for standardized boosters specifically timed for the transition to university life.
the development of multivalent vaccines—those that protect against a wider array of serogroups (strains)—will be essential as the bacteria evolves to bypass older vaccine protections.
The Psychology of Public Health Communication
When an outbreak hits a university town, panic often spreads faster than the disease. The “wider community concern” mentioned by experts highlights a gap in how we communicate risk.
The trend is moving away from top-down government announcements toward peer-to-peer health advocacy. By empowering student ambassadors to spread factual information about symptoms and prevention, universities can reduce stigma and anxiety while increasing vaccination uptake.
Transparent communication about “epidemiological links”—explaining that a few cases in a tight social group do not necessarily mean a city-wide epidemic—is key to maintaining public order and trust in health authorities.
For more information on current health guidelines, visit the World Health Organization or the NHS website.
Frequently Asked Questions
What are the early warning signs of meningitis?
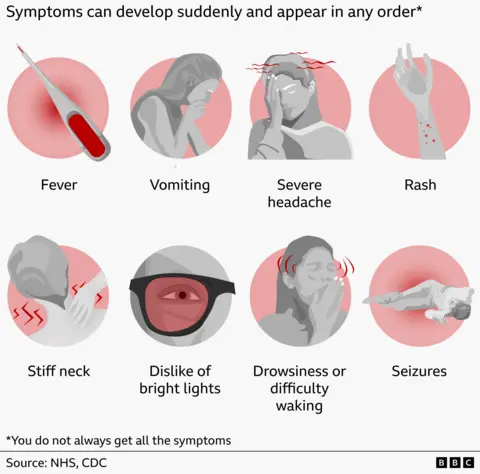
Symptoms often mimic the flu initially, including high fever and chills. However, the emergence of a severe headache, stiff neck, confusion, or a rash that doesn’t fade under pressure are red flags that require urgent medical attention.

Why are college students more susceptible?
High-density living (dorms), increased social mixing, and the stress of academic life can weaken the immune system and facilitate the spread of respiratory droplets, which is how the bacteria is transmitted.
If I’m not in a “contact group,” am I still at risk?
While the risk to the wider public is generally low during contained outbreaks, maintaining up-to-date vaccinations is the best defense for anyone living or working in high-density environments.
Join the Conversation
Are your campus health protocols up to date? Do you think digital contact tracing is a step too far, or a necessary evolution? Let us know in the comments below or subscribe to our newsletter for the latest in public health trends.