The Rise of Predictive Epidemiology: Forecasting the Next Outbreak
We are entering an era where we no longer have to wait for a patient to enter a clinic to know a crisis is brewing. By combining machine learning with satellite data, researchers are now mapping epidemic-prone diseases across nearly every country on Earth.
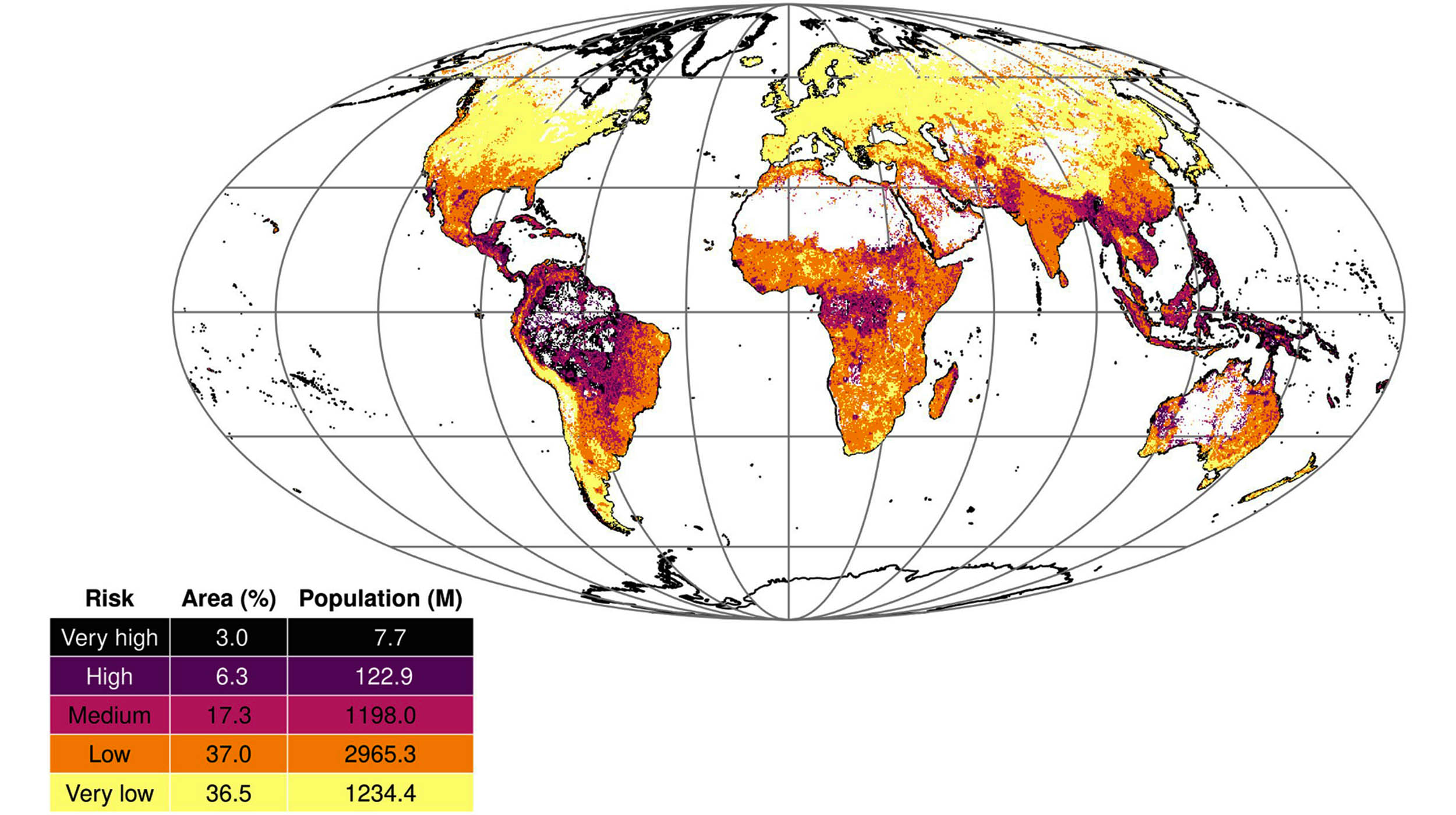
Recent global modeling reveals that approximately 9.3% of the world’s land area is highly vulnerable to dangerous disease outbreaks. Specifically, 6.3% is categorized as high-risk, while another 3% falls into the very high-risk bracket.
This shift toward predictive modeling, led by experts like veterinary epidemiologist Angela Fanelli at the European Commission’s Joint Research Centre (JRC), allows us to identify hotspots before they ignite. These tools analyze climate records, land utilize maps and past infections to narrow down where future threats might emerge.
The Climate-Disease Connection: Shifting Geographies
The geography of infectious disease is being rewritten by our changing environment. Warming air and water are altering the habitats where viruses, insects, and animals thrive.
Higher temperatures, deeper droughts, and heavier rainfall are all pushing outbreak risks upward. Longer warm seasons are particularly dangerous, as they allow disease-carrying ticks and mosquitoes to survive in new territories, pushing previously tropical infections into higher latitudes.
We can already see the real-world impact of environmental instability. Following Hurricane Melissa, regions in the Caribbean faced deteriorating epidemiological situations. In Jamaica, for instance, persistent flooding and disrupted water systems drove a confirmed leptospirosis outbreak and rising cases of tetanus, diarrhoeal illness, and dengue.
The Danger of “Spillover” Events
As human settlements expand into forests and wildlife markets, the resulting crowding increases the likelihood of “spillover”—the precise moment a virus crosses from an animal host into a human.

Clearing land for mines, roads, and farms brings people into closer contact with wildlife that host new pathogens. When biodiversity is lost, the remaining species that carry dangerous pathogens often find an advantage, further stacking the deck against human health.
The Human Factor: Population Density as a Primary Driver
While climate and land use are critical, the strongest driver of outbreak risk is population density. Packing large numbers of people and animals into dense settlements or industrial farms creates the perfect environment for viruses to jump and spread rapidly.
Currently, about 20% of the global population lives in medium-risk areas, while 3% inhabit zones of high or very high risk. These hotspots are heavily concentrated in Latin America and Oceania.
Bridging the Capacity Gap: Who is Ready?
The danger of an outbreak is not just about the likelihood of the virus appearing, but the capacity of the region to contain it. An “epidemic risk index” now combines outbreak likelihood with response capacity.
Some nations, such as the Republic of Congo and Papua New Guinea, face intense risk but possess limited health infrastructure. In these areas, clinics and laboratories may be quickly overwhelmed by a fast-moving outbreak.
Conversely, many high-income countries display low outbreak risk but maintain strong capacity. This creates an opportunity for these nations to serve as hubs for vaccine manufacturing and laboratory support for the more vulnerable regions.
Preparing for “Disease X”
The World Health Organization (WHO) maintains a priority list of dangerous zoonotic threats, but they also include a placeholder known as “Disease X.” This represents the unknown pathogens that have not yet emerged but could cause a future pandemic.

To combat this, agencies like Europe’s Health Emergency Preparedness and Response Authority are focusing on climate-sensitive threats such as Zika, Ebola, and Crimean Congo hemorrhagic fever.
The future of global health security lies in flexible preparedness: shared surveillance data, rapid financing, and adaptable vaccine platforms that can be pivoted the moment a new threat is detected.
Frequently Asked Questions
What is a zoonotic disease?
Zoonotic diseases are infections that move from animals to people through direct contact or infection.
Which regions are currently most vulnerable to outbreaks?
Hotspots are primarily concentrated in Latin America and Oceania, where climate change and land development pressures are highest.
What is “Disease X”?
Disease X is a placeholder term used by the WHO to encourage flexible preparedness for unknown future pathogens that could cause an epidemic.
What is the biggest driver of disease outbreak risk?
According to recent modeling, population density is the single strongest driver, outweighing individual environmental factors.
Stay Ahead of the Curve
Want to keep up with the latest in global health and environmental science? Join our community for deep dives into the trends shaping our future.