The Sweet Truth: How Sugar Intake Impacts Gallbladder Health
Recent research is shedding light on a surprising link between our diets and gallbladder health. A new study analyzing data from the National Health and Nutrition Examination Survey (NHANES) reveals a significant association between higher total sugar intake and an increased risk of gallstones in U.S. Adults. This finding underscores the growing concern about the impact of modern dietary habits on chronic disease development.
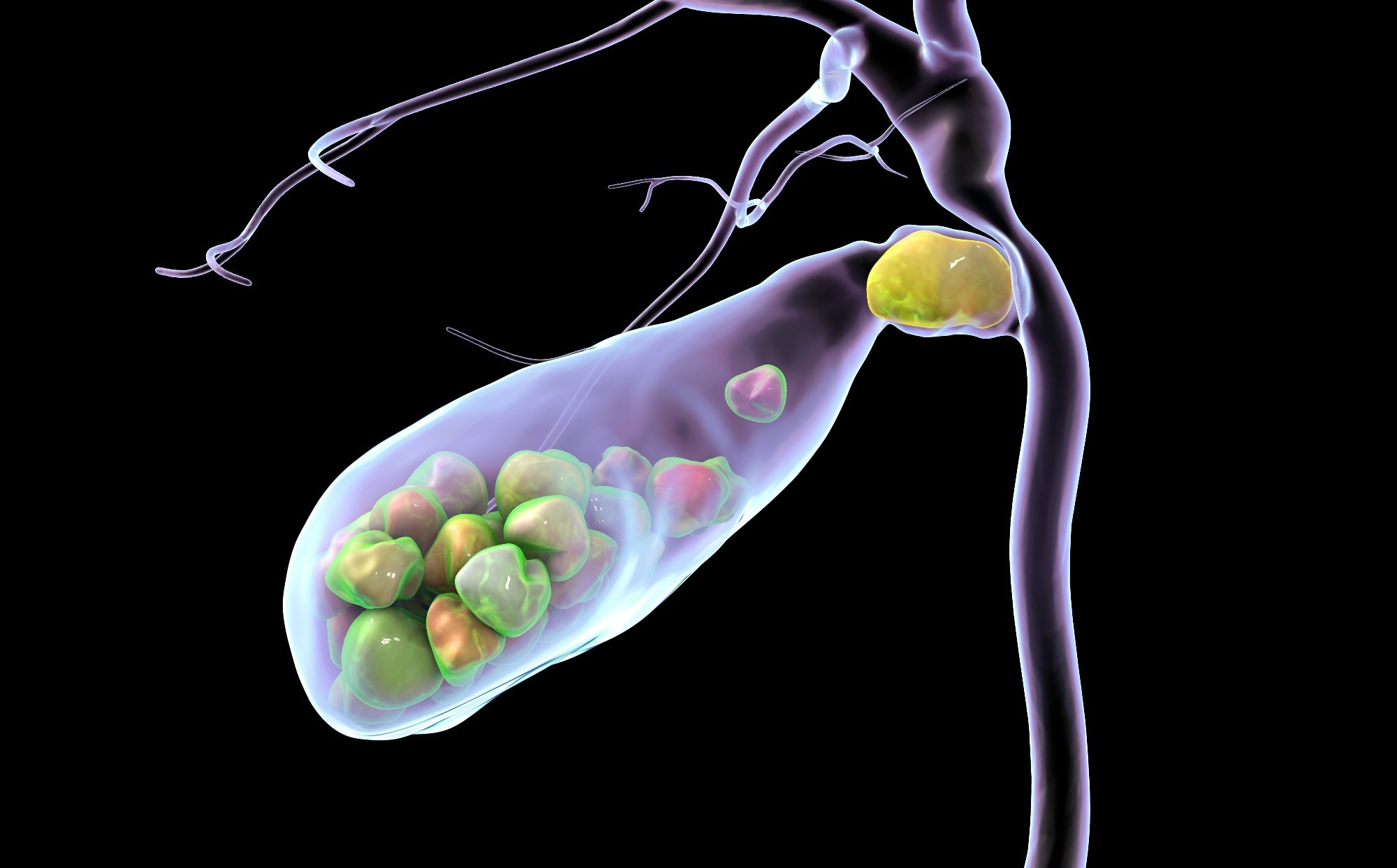
Gallstones: A Growing Health Concern
Gallstones are a common condition affecting the liver and biliary system. Their prevalence is rising globally, leading to complications like cholecystitis and pancreatitis, which contribute to substantial healthcare costs. Diet plays a crucial role in gallstone formation, and excessive sugar consumption is emerging as a key factor.
NHANES Data Reveals a Clear Connection
Researchers analyzed data from 8,975 participants in the NHANES survey (2017-2023). The study found that for every 100g/day increase in total sugar intake, the risk of gallstones increased by 41%, even after accounting for various lifestyle and dietary factors. Individuals consuming the highest amounts of sugar had an 82% higher risk compared to those with the lowest intake. This association remained consistent across different demographic groups.
The study employed sophisticated machine learning techniques, including XGBoost, to confirm sugar intake as a significant predictor of gallstone risk, ranking it sixth in importance behind age, gender, and BMI. The model demonstrated a high level of accuracy, with an AUC of 0.896.
How Does Sugar Contribute to Gallstone Formation?
The mechanisms linking high sugar intake to gallstone development are complex. Sugar, particularly fructose and sucrose, can alter bile composition and cholesterol metabolism. Increased blood glucose and insulin levels can lead to greater liver cholesterol production and secretion into bile, potentially causing supersaturation. High sugar diets may contribute to insulin resistance, obesity, reduced gallbladder motility, and bile stasis.
Emerging research suggests that excess sugar can also trigger oxidative stress and inflammation, impairing gallbladder function and accelerating cholesterol crystal formation. Disruption of the gut microbiota is another potential pathway, though further investigation is needed.
Sugar-Sweetened Beverages: A Major Culprit
Although the recent study focused on total dietary sugar, other research highlights the specific role of sugar-sweetened beverages (SSBs). A separate analysis of NHANES data (2017-2023) found that every 100 kcal/day increase in SSB consumption was associated with a 10% higher odds of gallstones. Consuming ≥300 kcal/day of SSBs was linked to an 81% higher risk. This relationship was found to be non-linear, suggesting that the risk increases disproportionately with higher SSB intake.
Future Trends and Research Directions
The growing body of evidence linking sugar intake to gallstone risk points to several potential future trends:
- Increased Public Health Awareness: Expect to see greater emphasis on reducing added sugar consumption in public health campaigns and dietary guidelines.
- Personalized Nutrition: Advances in genetic testing and microbiome analysis may allow for personalized dietary recommendations to mitigate gallstone risk based on individual susceptibility.
- Novel Therapeutic Approaches: Research into interventions targeting bile acid metabolism and gut microbiota modulation could lead to new therapies for preventing and treating gallstones.
- Food Industry Reformulation: Pressure on the food and beverage industry to reduce sugar content in processed foods and drinks is likely to intensify.
- Longitudinal Studies: Future research will focus on longitudinal studies to establish a causal relationship between sugar intake and gallstone development, and to better understand the underlying mechanisms.
Pro Tip
Read food labels carefully and be mindful of hidden sugars in processed foods. Opt for whole, unprocessed foods whenever possible.
Did You Know?
Gallstones can often be asymptomatic, meaning they don’t cause noticeable symptoms until complications arise. Regular check-ups and a healthy lifestyle are crucial for prevention.
Frequently Asked Questions
- What are the symptoms of gallstones? Common symptoms include sudden, intense pain in the upper right abdomen, nausea, vomiting, and jaundice.
- Can gallstones be prevented? Maintaining a healthy weight, eating a balanced diet low in added sugars, and staying physically active can help reduce your risk.
- Are there any medical treatments for gallstones? Treatment options range from medication to minimally invasive surgery, depending on the severity of the condition.
- Is fructose worse than other sugars? Research suggests that fructose may have a particularly strong link to metabolic disorders and liver problems, potentially increasing gallstone risk.
Reducing sugar intake is a simple yet powerful step towards improving gallbladder health and overall well-being. By making informed dietary choices, individuals can take control of their health and potentially reduce their risk of developing this common and often painful condition.
Want to learn more about gallbladder health? Explore our articles on liver detoxification and managing chronic inflammation.