The Great Medical AI Paradox: Proven Vision vs. Unproven Chatbots
Healthcare is currently navigating a strange contradiction. On one hand, we have “Deep Learning” AI—systems trained on millions of images that can spot patterns invisible to the human eye. On the other, we have “Generative AI” (LLMs), which are being adopted at lightning speed despite a significant lack of real-world clinical evidence.
For over a decade, AI has demonstrated “superhuman vision” in interpreting X-rays, CT scans, MRIs, and pathology slides. Yet, these validated tools often remain on the sidelines of standard medical practice. Meanwhile, millions of patients and physicians are turning to AI chatbots for diagnostic support, often bypassing the rigorous trial process that traditional medical tools require.
The Rise of Opportunistic AI: Finding What Wasn’t Sought
One of the most promising future trends is the shift toward Opportunistic AI
. What we have is the practice of using a medical scan ordered for one reason to screen for entirely different, unrelated conditions.
For example, in China, the PANDA tool is used to detect pancreatic cancer via chest and abdominal CT scans, even when the scan was originally ordered for a different issue. This transforms every routine scan into a comprehensive health screening, potentially catching deadly diseases years before symptoms appear.
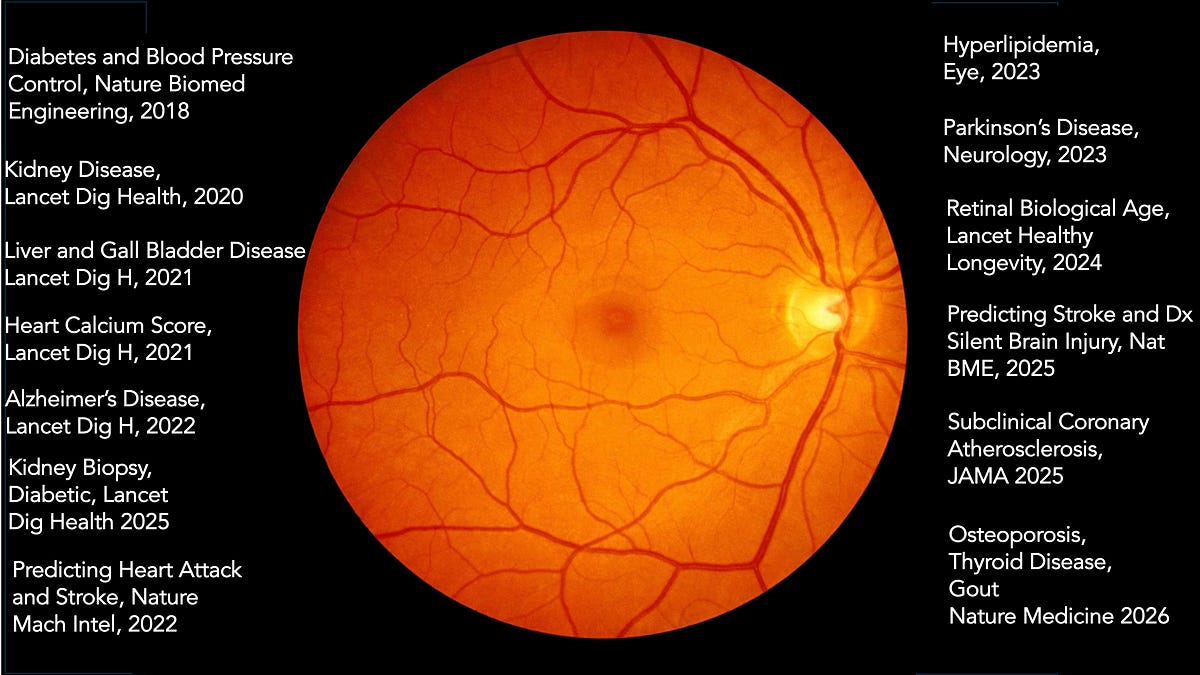
The Retinal Gateway to Total Body Health
The eye is effectively a window into the body’s vascular and neurological health. Foundation models like RETFound and Reti-Pioneer, trained on hundreds of thousands of images, are proving that the retina can signal risks for Type 2 diabetes, hypertension, and chronic kidney disease.
The future points toward a medical selfie
—the ability to capture a fundus image via smartphone and receive an instant AI readout of systemic health risks. This would decentralize diagnostics, moving them from the clinic to the palm of your hand.
From Chatbots to Clinicians: The Evidence Gap in Generative AI
While image-based AI is proven but underused, Generative AI is used but unproven. Recent data from the American Medical Association indicates that 72% of physicians use GenAI for at least one use case, with 35% applying it to direct, non-administrative patient care.
Still, the “real-world” data is thin. Many studies rely on simulations or case vignettes rather than actual patient outcomes. In some simulations, AI has even struggled with critical triage, making errors in high-stakes emergencies like respiratory failure or diabetic ketoacidosis.
Future Outlook: The Path to High-Performance Medicine
To move toward truly high-performance medicine
, the industry must bridge the gap between innovation and implementation. This requires a two-pronged approach: accelerating the adoption of proven imaging AI and demanding rigorous, randomized controlled trials (RCTs) for LLMs.
We are seeing the beginning of this shift. Recent studies in Science Magazine and Nature Medicine are calling for a move away from simulations and toward prospective clinical trials with independent adjudication of health outcomes.
The goal is a hybrid ecosystem where the “vision” of deep learning and the “reasoning” of LLMs work in tandem, overseen by a human-in-the-loop to ensure safety and accuracy.
Frequently Asked Questions
Can AI completely replace my doctor for a diagnosis?
No. While AI can outperform humans in specific tasks (like spotting a polyp during a colonoscopy), it lacks the holistic judgment and physical examination capabilities of a physician. The future is “AI-assisted” medicine, not “AI-only” medicine.

What is the difference between Deep Learning and Generative AI in medicine?
Deep Learning (DL) typically refers to pattern recognition, such as identifying a tumor in an MRI. Generative AI (like ChatGPT) refers to models that can process language and reason through a problem to generate a response or plan.
Is it safe to use AI chatbots for health information?
They are excellent for preparing questions for your doctor or understanding a diagnosis in simpler terms. However, they can “hallucinate” or miss critical emergency signs, so they should never be used as a sole source for emergency triage or treatment changes.
Join the Conversation on the Future of Health
Are you a healthcare provider using AI in your practice, or a patient who has tried AI for health support? We want to hear your experience.
Exit a comment below or subscribe to our newsletter for the latest updates on medical technology.