The “Identity Crisis” of Cancer: Redefining Hodgkin Lymphoma
For years, medical science viewed Hodgkin lymphoma primarily through the lens of uncontrolled cell growth. However, groundbreaking research from Weill Cornell Medicine is shifting that narrative. We now understand that these cancer cells are actually immune cells experiencing a profound “identity crisis.”
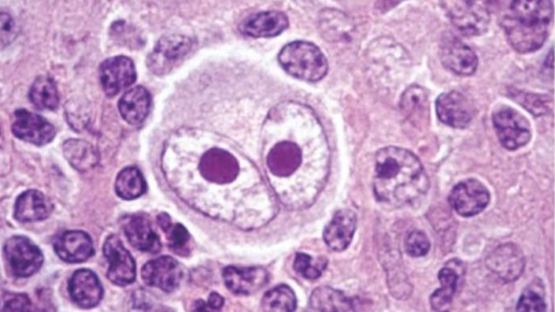
Normally, a B cell matures into a plasma cell to produce antibodies that fight infection. In patients with Hodgkin lymphoma, this process is aborted. The cells are trapped partway through the transition, switching off B cell features but failing to become functional plasma cells. These stalled cells become malignant, known as Reed-Sternberg cells.
Precision Diagnostics: The Rise of New Biomarkers
One of the most significant future trends in treating blood cancers is the move toward high-precision diagnostics. Because Hodgkin lymphoma cells resemble plasma cell cancers—like multiple myeloma—more closely than other lymphomas, researchers are identifying specific markers to tell them apart.

A key focus is the PDIA6 protein. Because this protein is specifically upregulated in Hodgkin lymphoma cells as part of their unique stress response, it may serve as a critical diagnostic biomarker. This allows physicians to distinguish Hodgkin lymphoma from related non-Hodgkin lymphomas more accurately, ensuring patients receive the correct treatment plan from the start.
Targeting the Survival Mechanism: The UPR Pathway
The future of lymphoma therapy is moving away from broad-spectrum chemotherapy, which often carries long-term side effects, toward targeted molecular therapies. The discovery of the unfolded protein response (UPR) pathway provides a new target.
In healthy plasma cells, the UPR helps the cell handle the stress of producing massive amounts of immunoglobulins. Since Hodgkin lymphoma cells cannot produce these antibodies but still activate the UPR, they use this pathway as a survival mechanism to manage internal strain.
By selectively targeting the UPR, future treatments could potentially “starve” or destabilize the cancer cells without damaging healthy tissue, offering a more refined alternative to traditional radiation and chemotherapy.
Breaking the Cloak: Overcoming Immune Evasion
A major hurdle in treating Hodgkin lymphoma is the cancer’s ability to hide from the immune system. Research has revealed that these cells employ a sophisticated “cloaking” strategy to evade both the innate and adaptive immune responses.
- NK Cell Evasion: Hodgkin lymphoma cells downregulate SLAM-family ligands, such as CD48. This prevents natural killer (NK) cells from recognizing the tumor as a threat.
- Active Exclusion: Evidence suggests the tumor may actively repel or exclude NK cells from the tumor site.
- T Cell Escape: The cells use additional mechanisms to bypass T cell detection, effectively escaping the two primary arms of immune surveillance.
Future therapeutic trends are likely to focus on “unmasking” these cells, potentially by restoring the expression of markers like CD48, allowing the body’s own immune system to identify and destroy the malignancy.
The Path Forward in Hematologic Malignancies
The collaboration between institutions like Weill Cornell Medicine, Memorial Sloan Kettering Cancer Center, and NYU Langone Health highlights a trend toward multi-institutional research to tackle blood cancers. By analyzing gene expression profiles across primary tumors and cell lines, researchers are uncovering the molecular blueprints of these diseases.

This shift from treating the symptoms of “uncontrolled growth” to addressing the “failure of cell development” opens the door for a new generation of therapies that treat the root cause of the malignancy.
For more information on current research and available options, you can explore the Weill Cornell Lymphoma Program or browse open clinical trials for lymphoma.
Frequently Asked Questions
What are Reed-Sternberg cells?
They are the malignant cells found in the lymph nodes of people with Hodgkin lymphoma, characterized by an “owl eye” appearance and a failed transition from B cells to plasma cells.
How does Hodgkin lymphoma differ from non-Hodgkin lymphoma?
While both affect the lymphatic system, Hodgkin lymphoma is specifically characterized by the presence of Reed-Sternberg cells and a distinct genetic profile that more closely resembles plasma cell cancers.
What is the UPR pathway?
The unfolded protein response (UPR) is a cellular stress response. In Hodgkin lymphoma, it is used as a survival mechanism by cancer cells that cannot produce antibodies.
Who is most affected by Hodgkin lymphoma?
It is the most common cancer in adolescents aged 15–19, though it also frequently affects adults over the age of 55.
Join the Conversation: Do you suppose targeted molecular therapies will eventually replace traditional chemotherapy for blood cancers? Share your thoughts in the comments below or subscribe to our newsletter for the latest updates in oncology research.